-

Ability of Video Telemedicine to Predict Unplanned Hospital Readmission for Single Ventricle Infants
Doaa Aly, Lori Erickson, Hayley S. Hancock, Johnathan Apperson, Kimberly J. Reid, Jennifer A. Marshall, Girish S. Shirali, and Suma Goudar
Background:
Our Cardiac High Acuity Monitoring program (CHAMP) utilizes daily videos as an adjunct to monitor interstage single ventricle infants (SVI) at home. The current study was designed to develop and validate an objective clinical scoring system for video analysis, in order to identify SVI at risk for clinical deterioration and predict unplanned hospital admissions (UHA).
Methods:
Six candidate items (respiratory rate and effort, color, behavior, skin and general appearance) were selected using local expert consensus to develop a pragmatic score for standardized video analysis. Observations were scored from 0 to 2 or 4, with higher numbers for increasing levels of concern. Thus, respiratory rate was graded 0-4 with increasing scores for increasing tachypnea or bradypnea. Respiratory effort was graded based on retractions and perceived use of accessory muscles. Color was graded as pink, pale and gray. Behavior was graded as appropriate, somnolent or irritable. Skin was dichotomous for the presence or absence of rash and/or infection. Appearance was graded as expected, mild concern or significant concern.
All SVI monitored at home by CHAMP between March 2014-March 2018 at our center were included. The primary outcome variable was UHA. Videos obtained within 48 hours prior to UHA (case videos) were compared to videos obtained at baseline (control videos). A subset of 30 videos was reviewed by a second blinded rater for inter-rater reproducibility. Independent t-, paired t- and Mcnemar’s tests were used for comparisons. Inter-class coefficients (ICC) were used to quantify reproducibility. Receiver operating characteristic (ROC) curve was used to establish a cut off score for predicting UHA.
Results:
Thirty-nine subjects with 64 UHA were included. We compared 64 case videos to 64 paired controls. Video scoring was feasible for 91.6% of all observations with 64 non scorable- items, due to inadequate lighting, distance or clothing. Of those, 16 were for skin. ICC for inter-reader reproducibility of video score items ranged from 0.73-0.98. Individual score items were significantly higher in case videos than in controls, with the exception of skin scores. Hence, skin was removed from the total video score. The resulting 5-item video composite score provided values ranging from 0 to 15. Mean composite scores were significantly higher for cases (6.9 ± 2.1) than for controls (1.7 ± 1.3), P< 0.001. Area under the ROC curve was 0.97. Score of 4.5 provided sensitivity of 89% and specificity of 97% to predict UHA.
Conclusion:
We developed a reproducible video telemetry score that can serve as a tool to predict UHA in SVI. Future directions involve prospective, multicenter validation of this tool.
-

Association of Enteral Tube Feedings at Discharge for Neonates with Critical Congenital Heart Disease
Lori Erickson, Katherine Bonessa, Usman Hasnie, Janelle R. Noel-Macdonnell, Natalie Jayaram, Julie Weiner, and Tara Swanson
Background: Infants with critical congenital heart disease (cCHD) are at risk for requiring supplemental enteral nutrition or tube feedings (TF). We sought to determine clinical characteristics associated with requirement for nasogastric or gastric tube feedings at neonatal discharge following surgery for cCHD.
Methods: We retrospectively reviewed data from all newborns with cCHD requiring cardiac surgery within the first 30 days of life (n=377) from our tertiary children’s hospital (CH) from January 2008 to March 2013. Descriptive statistics PO vs. TF comparisons using a univariate analysis were completed. Multivariable logistic regression with variable receiver operating characteristics (ROC) curve comparisons were used to determine the association between patient characteristics and requirement for TF at discharge. Patients who did not survive to discharge were excluded from this secondary analysis.
Results: Of 339 neonates, 122 (36%) were discharged with TF (67 PO+NG, 19 PO+GT, 36 GT). Univariate analysis: when compared to those that were fed orally, TF infants had similar prenatal detection (37.7% vs 42.4%, p=0.40), single ventricle palliation (37.7% vs 37.8%, p=0.99), and STAT scores (69.5% STAT ≥ 4 vs 66.8%, p=0.37). In contrast, lower incidence of pre-operative feedings (62.3% vs 73.3%, p=0.04), higher rate of sepsis (23.8% vs 8.8%, p < 0.001), and higher rate of necrotizing enterocolitis (NEC) (15.6% vs 4.1%, p < 0.001) were noted with TF infants. After multivariable adjustment, no associations persisted between TF and pre-operative feeding, sepsis, or NEC. The odds of TF increased with distance from the CH and birth hospital [estimate 1.07 per 20 mile distance from CH; 95% confidence interval (CI) 1.016, 1.129, p=0.01] or increase of 7% risk TF for every 20 miles. The odds of TF increased with 2 or more subspecialty consults [Odds Ratio (OR) 3.18; 95% CI 1.75, 5.78, p < 0.001] and major genetic abnormalities (OR 2.82, 95% CI 1.28, 6.39, p=0.01). Delays in post-operative feedings were associated with higher likelihood of need for enteral nutrition (estimate 1.12; 95% CI 1.05, 1.20, p < 0.001), indicating a 12% increase for each day delay in post-surgical feeding.
Conclusions: Infants with cCHD that deliver farther from the children’s hospital, have multiple subspecialty consults, genetic abnormalities, and delays in post-operative feeds are associated with a greater likelihood for tube feeds at hospital discharge. A probability model was fit to this current data set. This model will continue to be tested and validated to predict tube feedings in new patients.
-

Crk/CrkL- Mediated Regulation of Cell Cycle Genes in Fibroblasts
Giridhar Mudduluru, Tom Curran, and Taeju Park
CT10 regulator of kinase (Crk) and Crk-like (CrkL) are cytosolic adaptor proteins that play important roles in cell proliferation, adhesion, and migration. In addition, Crk and CrkL are structurally similar to each other and play essential overlapping functions. Crk and CrkL are also known to be overexpressed in non-small cell lung cancer, ovarian, gastric and glioblastoma cancers and have been suggested as novel therapeutic targets for cancer treatment. Ablation of endogenous Crk and CrkL from cultured fibroblasts carrying floxed alleles of Crk and CrkL by transfecting with synthetic Cre mRNA resulted in a failure of cell proliferation and cell cycle arrest at the G1-S transition. To elucidate the mechanism of Crk/CrkL-mediated functions, we performed custom RT2 profiler PCR arrays after conditionally ablating both Crk and CrkL from fibroblasts. Loss of Crk and CrkL led to significant changes in expression levels of cell cycle genes such as cyclin D1. In addition, non-coding RNAs such as miR-1a-3p, miR-23b-3p, miR-99a-5p, and miR-335-5p, which are known to reduce cell proliferation and tumor metastasis, were up-regulated in the absence of Crk and CrkL. Changes in the expression levels of miR-335-5p and cyclin D1 were confirmed by q-PCR and Western, respectively. Additionally, Western blot analyses showed that loss of Crk/CrkL from cells increased the expression of p27Kip1. Reintroduction of CrkII restored the cyclin D1 expression and repressed the p27Kip1 expression. Our results suggest that Crk and CrkL control the cell cycle by regulating gene expression of cyclin D1, p27Kip1 and miR-335-5p. With these results, we are extending our study to cancer models to gain clear knowledge on biological functions of Crk/CrkL in cancer.
-
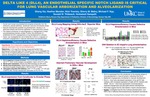
Delta Like 4 (DLL4), an Endothelial Specific NOTCH Ligand is Critical for Lung Vascular Arborization and Alveolarization
Sheng Xia, Heather Menden, Nicholas Townley MD, Sherry M. Mabry, Michael F. Nyp, Donald W. Thibeault, and Venkatesh Sampath
Background: Defective vascular development is a hallmark of bronchopulmonary dysplasia (BPD) of prematurity. Mechanistic regulation of normal and abnormal vascular development in the saccular/alveolar lung remain incompletely understood. To investigate the role of the endothelial cell (EC) in distal lung vascular arborization and alveolarization (the vascular hypothesis), we targeted Delta like 4 (DLL4), an EC Notch ligand, and master regulator of embryonic angiogenesis, hypothesizing that DLL4-dependent angiogenesis is critical for arborization and alveolarization.
Objectives: i) to map DLL4 and angiogenesis signatures from the canalicular to alveolar phase (human/mouse lung development), and ii) to examine the effect of Dll4 (Dll4+/LacZ) haploinsufficiency and EC-specific Dll4-deletion on lung vascular and alveolar development.
Design/Methods: Immunofluorescence staining and confocal microscopy of DLL4 (EC tip cell marker), JAG1 (EC stalk cell marker), and PECAM on mouse and human lung (autopsy), from canalicular to alveolar phase was performed. In Dll4+/LacZ mouse sections, Dll4 expression pattern was assessed with X-gal staining. Vascular development and alveolarization were assessed via PECAM staining, radial alveolar counts (RAC) and mean linear intercepts (Lm). Tamoxifen inducible, EC specific knockout mice (Dll4 Loxp/Loxp; Cdh5-CreERT2) were used to examine DLL4’s alveolar phase role.
RESULTS: DLL4 was expressed in mouse lung from E17 to P28; in human, 23-43wks gestation, with peak expression in alveolar phase, in small arteries and capillaries, in a PECAM-restricted manner. Stalk cell marker (JAG1), and EC Notch activation (NICD) mirrored and approximated EC DLL4 expression in mouse and human. Lung Dll4 (X-gal) expression was confirmed from E17 to P28 using Dll4+/LacZ mice, with prominent expression in the saccular/early alveolar phase and in secondary septa. Dll4 haploinsufficiency (Dll4+/LacZ) resulted in hyper-sprouting of lung vessels (E17), disorganized capillaries (P6), and narrowed-lumen capillaries and smaller intermediate vessels (P14). Dll4+/LacZ mice had defective alveolarization (decreased RAC and increased Lm). Inducible-deletion of EC Dll4 before alveolar phase (P4, P5) disrupted alveolar development in mid-alveolar phase (P14).
CONCLUSIONS:Dll4-dependent angiogenesis regulates lung vascular development. Loss of one or two copies of Dll4 impairs angiogenesis, disrupting alveolarization. Our data evince a direct role for EC-Dll4 in regulating alveolarization and inform Dll4 investigation as a prime candidate for defective vascularization and alveolarization in BPD (bronchopulmonary dysplasia).
-

Development and Implementation of a Hydration Protocol for Cystic Fibrosis Patients Receiving Nephrotoxic Medications
Stephanie Duehlmeyer, Claire Elson, and Hugo Escobar
BACKGROUND:
A risk factor for the development of acute kidney injury (AKI) in hospitalized patients is exposure to nephrotoxic medications (NTMx). Cystic fibrosis (CF) patients admitted for pulmonary exacerbations (PEx) are commonly exposed to NTMx. There is limited data on the development, implementation and outcomes of a hydration protocol (HP) for CF patients admitted for a PEx to prevent AKI.
METHODS:
An electronic survey was submitted to 13 providers at Children’s Mercy Kansas City (CMKC) and the CF pharmacist listserv to gather baseline interest and center practices. Based on the survey results and evaluation of published literature, a standard HP was developed to be utilized for all CF patients admitted for a PEx. Baseline exposure rates to NTMx and AKI rates were analyzed from January 2017 to July 2017. The HP was implemented in July 2018. Post-implementation data was analyzed from July 2018 to February 2019. AKI rates were evaluated while on NTMx defined as ≥50% increase from baseline (admission SCr) or an absolute increase of 0.3 mg/dL within 48 hours. The hydration protocol entails initiating IV fluids for the first 48 hours while on NTMx and includes a consult to Child Life to make individualized fluid charts.
RESULTS:
All 10 (77%) respondents to the CMKC survey supported the implementation of a standardized HP. Prior to HP implementation, 45 individuals were exposed to NTMx comprising an exposure rate of 54.48 and an AKI rate of 7.26 per 1000 non-ICU days. Post-implementation of the HP, 61 individuals were exposed to NTMx with an exposure rate of 58.15 and AKI rate of 6.67 per 1000 non-ICU days. The mean duration of AKI was 1.17 ±0.41 days pre-implementation compared to 1.57 ±0.98 days post-implementation. The most common NTMx associated with AKI were tobramycin, vancomycin, colistimethate and piperacillin/tazobactam. There were 14 (23%) HP deviations primarily because the individuals did not receive intravenous fluids for 48 hours while on two NTMx. Of 61 encounters, 32 (52.5%) declined a fluid chart. Of those 32 encounters, 6 (19%) developed AKI, while only 1 (3%) individual that utilized a fluid chart developed AKI.
CONCLUSIONS:
Implementation of the HP decreased AKI rate of CF patients admitted for PEx while receiving NTMx. This data demonstrates a need for a larger study over a longer duration and suggests the potential need for a standardized HP for patients exposed to NTMx hospital-wide.
-

Documenting Training Using REDCap
Carol Claro, Robin E. Ryan, and Keith August
Background: ICH Guidelines for Good Clinical Practice (GCP) states, “Each individual involved in conducting a trial should be qualified by education, training, and experience to perform his or her respective task(s).” Systemizing and documenting staff training for multi-disciplinary trials is challenging.
Purpose: Prior to 2018, documentation of training at Children’s Mercy was not captured in a systematic manner. The COG team wanted to identify a platform for distributing and tracking completion of training materials for study team members. REDCap is a secure web application that can be used to build and manage online surveys. The purpose of this effort was to determine if REDCap could effectively document training.
Methods: In 2017, COG regulatory effort was consolidated into one position. The Regulatory Coordinator (RC) is responsible for maintaining documentation of protocol training. Prior methods in achieving this were inconsistent. In 2018, after discussion and trials, training for new protocols and amendments were forwarded as a REDCap survey to study team members. Recipients are asked to review the modules and attest to understanding with a date and signature stamp. The REDCap dashboard provides the PI and RC a tool to view completion. The system allows automatic email reminders to be sent to any delinquent team members.
Results: REDCap provides a platform for protocol training, communication and real-time tracking.
Conclusions: Attributes for good documentation as described by US-FDA are attributable, legible, contemporaneous, original and accurate (Bargaje, 2011). REDCap creates an audit trail of documentation reflecting compliance with GCP.
-

Factors Associated with Length of Stay and Transfer Rates in the Pediatric Urgent Care Setting: 2017 OUCH Data
Meghan Cohen, Brian Lee, and Amanda Montalbano
Purpose: Urgent Care (UC) currently represents a heterogeneous population of clinic sites with varying staffing and care models. The goal of the study was to explore factors associated with patient length of stay (LOS) and disposition of transfer.
Background/Significance: Urgent Care centers are one of the fastest growing venues of health care delivery. Due to the share of pediatric patients seen in UC, there has been a growth of specialized pediatric UC centers. Pediatric UC centers have not been studied in terms of practice variation or patient outcomes because there is no centralized database to study these patients. To define common administrative practices of pediatric urgent care: staffing, scope of practice, and ancillary services as well as clinical measures such as patient throughput, disposition of transfer, and length of stay.
Methods: This is a cross-sectional national survey of pediatric urgent care sites. Contributing sites were recruited from national professional organizations of pediatric urgent care providers. The online survey was administered and collated into a REDCap database. Counts and frequencies were used to analyze the categorical data. Continuous data were described with median and interquartile ranges. Non-parametric distributions in LOS, transfer rates, and throughput were compared using Mann-Whitney U tests and Spearman’s correlation was used to describe dependency of variables.
Results: From emailed invitations, 125 of the 188 sites (66%) completed the survey. Slightly more than half (55.2%) were associated with a hospital system; whereas, the other 44.8% were privately owned. The median annual patient volume was 12594 [7719, 20664] and length of stay was 56 minutes [48, 73]. There was a correlation (r=.28, p=0.01) of increasing volume with increasing LOS, although this may not be clinically significant. There was no correlation (r=0.12, p=0.31) between LOS and throughput (patients per provider per hour). Median transfer rate was 1.6% [1-3.9%]; however, there was significant difference in transfer rates between hospital based (2.8%) and privately owned (0.7%) pediatric urgent care centers.
Conclusions: Increasing expertise and scope of care was correlated with decreased LOS. Transfers were less likely in a privately owned pediatric urgent care, but overall were positively associated with increasing LOS. Future studies on clinical outcomes and quality of care in relation to LOS and transfer rates are needed.
-

Food Cost of Classic Ketogenic Diet in Patients With Glut1
Rachel Finn, Lindsey Thompson, Rhonda Sullivan, and Erin Lindhorst
Introduction: Glucose Transporter Deficiency Syndrome (GLUT1) is a rare genetic metabolic disorder characterized by deficiency of a protein that is required for glucose to cross the blood-brain barrier. The current gold standard treatment for GLUT1 is the ketogenic diet (KD). The KD is carefully tailored to individual patients and involves purchasing specific foods unique to the family member on the KD. The foods and supplements required on the KD are currently an out of pocket expense for the majority of families (minimal insurance coverage). A review of literature indicated the average cost of the specialty foods and supplements to families is unknown. The purpose of this study was to determine the estimated monthly cost of KD ingredients of foods and supplement consumed by orally fed patients with GLUT1.
Methods: This study involved a retrospective chart review of patients seen in the Epilepsy Center at Children’s Mercy Hospital (CMH) with the diagnoses of GLUT1 between 4-24 years of age who wereorally fed on the classic KD. These patients are on the medically prescribed classic ketogenic diet which provides the recommended energy for their diagnosis. Patient’s current meals, snacks and supplements were analyzed for the cost of the ingredients the families purchase. Cost of the ingredients was determined through visits to local grocery stores,averaged and then used for the calculations. The use of a ketogenic diet calculation program was used to determine the total grams of ingredients the patients consumed through pre-calculated meals, snacks and supplement for each patient. Calculation parameters include age, gender, diet ratio and calories were compared to the USDA food plans: Cost of Food at Home at the liberal plan for a family of four.
Results: Nine patients with GLUT1 were identified on the KD at CMH. Average monthly cost of foods purchased was $143-185 per patient on the KD compared to USDA estimated average monthly cost food plan for a family of four $42-82. Average cost was not associated with age, gender, calories nor ratio. Cost of ingredients reflected on the types of foods the patient consumed. Micronutrient supplement costs ranged between $0.22-2.22 per day per patient.
Conclusion: The average cost of ingredients for GLUT1 patients on the KD is 1.75-3.5 times greater than the USDA average for age/gender for a liberal food plan. TheKDfoods and supplements are currently an out of pocket expense for mostfamilies. Future research will include multiple sites representing additional regions of the United States. The data collected can provide information for potential future legislation or program development intended to support families’ expenses related to the dietary treatment of their disease.
-

Functional Consequences of Pravastatin Isomerization on OATP1B1-Mediated Transport
Jonathan B. Wagner, Melissa Ruggiero, J Steven Leeder, and Bruno Hagenbuch
Background: Pravastatin (PVA) is subject to pre-systemic conversion to an inactive isomer, 3’α-iso-pravastatin acid (3αPVA), in the acidic environment of the stomach. Inter-individual differences in the relative amounts of circulating PVA and 3α-PVA have been observed in adults and confirmed in children. Our previous investigation in children suggested that 3αPVA was a substrate of OATP1B1, but additionally a possible competitive inhibitor of OATP1B1.As a consequence, PVA concentrations at the site of drug action in the liver may be reduced further, potentially compromising efficacy.
In the present study, we examined the functional consequences of 3α-PVA on OATP1B1-mediated PVA transport and whether it is a competitive inhibitor of OATP1B1.
Methods: Site directed mutagenesis was performed to generate SLCO1B1 genotypes of interest (*1a, *1b, *5, *15). Human embryonic kidney (HEK293) cells were grown and plated at 200 000 cells per well in 24-well plates. Twenty-four hours later the cells were transfected with the aforementioned plasmids. Forty-eight hours later cell-based transport was performed with radiolabelled [3H]-pravastatin sodium salt. Non-radioactive pravastatin sodium salt and 3’α-iso-pravastatin sodium salt was used for PVA transport and 3αPVA studies, respectively. Data were analyzed for significant differences amongst genotype groups using ANOVA followed by Tukey’s multiple comparisons test. IC50 and kinetic parameters were calculated using non-linear regression analysis.
Results: Pravastatin transport in SLCO1B1 variants (*5,*15) was significantly decreased compared to the reference genotype *1a and *1b (Km [µM]: *1a 18.2±0.9; *1b 17.9±3.3; *5 34.2± 9.7; *15 34.1±6.1; p≤0.05; Vmax [pmol/mg/min]: *1a 104.9±13.1; *1b 93.7±16.7; *5 44.8±15.9; *15 62.3±22.5; p≤0.05). *1a and *1b were not significantly different with respect to pravastatin transport. Intrinsic clearance was diminished nearly 4 to 5-fold in SLCO1B1 variants compared to reference genotypes (Vmax/Km [µl/min/mg]: *1a 5.8 ± 0.8; *1b 5.7 ± 1.9; *5 1.3 ± 0.2; *15 1.8 ± 0.3; p≤0.01).
Pravastatin transport was inhibited by 3αPVA for all genotypes. However, there was more pronounced inhibition in the SLCO1B1 variant genotypes compared to reference genotypes (IC50 [µM]: *1a 15.9±1.9; *1b 18.6±5.7; *5 3.9±2.0; *15 4.4±0.8; p≤0.01).
Discussion: The functional consequences of 3αPVA formation on PVA transport was confirmed in our study. Mechanistically, we confirmed our observation in humans that 3αPVA inhibits OATP1B1 transport. However, this effect is more pronounced in variant genotypes as shown by lower IC50 values compared to the reference genotypes. This highlights another source of variation that must be taken into consideration when trying to optimize the pravastatin dose-exposure relationship in humans.
-

Improved Vitamin D Status Over Time in Children Undergoing Hematopoietic Cell Transplantation
Nancy Shreve, Rakesh Goyal, Vincent S. Staggs, Katrina Walters, Jos Domen, Jean Freundenthal, Uttam Garg, Nancy Green, Rukhsana Rahmetulla, Nancy Terwilliger, Mohamed Radhi, and Jignesh Dalal
BACKGROUND: Vitamin D deficiency is prevalent in children undergoing hematopoietic cell transplantation (HCT), and has been correlated with risk of post-transplant complications and inferior survival. We report findings from a prospective non-interventional study of vitamin D status over time in pediatric HCT patients.
METHODS: Patients between >1 mo. and ≤21 y age were eligible. Blood samples were drawn to measure 25-hydroxy vitamin D (“vitamin D”) levels at pre-HCT, and 100 days, 6 mo., 1 y, and 2 y post-HCT timepoints. Vitamin D levels were classified as sufficient ( ≥ 30 ng/ml), insufficient (20–29 ng/ml) or deficient ( < 20 ng/ml). All patients were followed by registered dieticians. Logistic mixed models were used to examine vitamin D status across time.
RESULTS: Sixty-six patients were enrolled, median age 8.1 y (0.4 y -20.5 y). 73% of patients received myeloablative conditioning. The median vitamin D level prior to HCT was 27 ng/ml (range: 8 ng/ml – 69 ng/ml). Levels were insufficient and deficient in 33% and 23% patients (Table 1). Only 24% of children > 12 y had sufficient vitamin D levels compared with 44% and 64% in in ages 4-12 and below 4 y respectively. Only 24% female patients had normal vitamin D levels compared with 45% male patients. Vitamin D sufficiency rates were similar between whites and non-whites. Compared to pre-HCT, estimated odds of “below sufficient” (either insufficient or deficient) were 47% higher at 100 days, 30% higher at 6 mo., 69% lower at 1 y, and 81% lower at 2 y (linear trend p = .023) and estimated odds of sufficiency were 39% lower at 100 days, 21% lower at 6 mo., and 41-42% higher at 1 y and 2 y (linear trend p = .087)(Figure 1). A review of medical records showed that proportion of patients receiving supplemental vitamin D were 7.5%, 10%, 19%, 30% and 42% at pre-HCT, +100 days, 6 mo., 1 and 2 y post-HCT time-points, respectively.
CONCLUSIONS: We show a high prevalence rate of vitamin D insufficiency and deficiency prior to and early after HCT. We also found that the odds of vitamin D sufficiency improved over 1 – 2 y post-HCT. We recommend that all pediatric patients should be screened for vitamin D status prior to and at day 100 post-transplant and those with low levels ( <2 0 ng>/mL) treated. Clinical significance of this approach needs to be examined in a large multicenter trial.
-

Lidocaine Infusion for Pediatric Pain: Initial Experience Beyond the OR
Elizabeth Edmundson, Lynn Anson, Heather Miles, Shannan Orpin, Vincent S. Staggs, and Daniel L. Millspaugh
Introduction: Intravenous (IV) lidocaine is increasingly part of inpatient multimodal analgesia. Little pediatric literature exists regarding its use beyond the OR; we describe our initial experience.
Methods: Cases from 1/2016 to 7/2018 were retrospectively reviewed. Four groups were defined: Sickle cell/VOE, Post-op, Cancer, and Other. Lidocaine infusion initiation was defined as on Day 0. Plasma concentration (Cp) goal was 2-4 mcg/ml per policy. Data were presented graphically, and linear mixed models were also used to estimate trajectories for average daily pain score and opioid use, in Morphine Milligram Equivalents (MME), with age and post-op days as covariates.
Results: Table 1 shows demographics and mean infusion characteristics. Seven treatments (23%) included an initial bolus. Six infusions (20%) were stopped on Day 0, two for Cp ≥ 10 mcg/ml. One of these patients subsequently had a seizure coincident with a transfusion-related fever (Cp ≤ 5.6 mcg/ml). Paresthesia occurred in 20%. Figure 1 shows the lowest pain scores and MME recorded as percent change from baseline (Day 0 for Post-op, Day -1 otherwise). Figures 2 and 3 show pain score and MME trajectories. Based on modeling, MME decreases, on average, by an estimated 12% (95% CI: 4%-20%) and 13% (95% CI: 3%-21%) per day, in Cancer and Other groups, respectively (p = .006, .011). Pain scores for Cancer patients decrease by an estimated average of 0.7 (95% CI: 0.4-1.0) per day (p < .001).
Discussion: The exact analgesic mechanism of systemic lidocaine is not known, but it may involve anti-inflammatory effects and NMDA receptor modulation. It is not unexpected then that greatest benefit was in the Cancer and Other groups, which included mucositis, typhlitis, colitis, metastasis, and nerve injury. Careful assessment of hepatic blood flow, metabolic factors, and cardiac and neurologic history is a must, with infusion rate adjusted accordingly.
Conclusions: IV lidocaine lowered pain scores and opioid use most in inflammatory and neuropathic pain.
-

Maternal Cigarette Smoke Exposure Induces Alterations in the Transcriptome and Methylome of Human Placenta
Carrie A. Vyhlidal, Abby Kietzman, Warren A. Cheung, Jeffrey J. Johnston, Adam Walter, Rebecca L. Biswell, and Elin Grundberg
Maternal cigarette smoke exposure (CSE) continues to be a common prenatal exposure with approximately 10% of babies exposed in uteroduring the third trimester in the U.S. and is the predominant risk factor for having an infant that is small for gestational age (SGA). Cigarette smoke is a complex mixture of thousands of chemical compounds that may directly affect the developing fetus or indirectly affect growth by disrupting placenta development and function. The individual components of maternal cigarette smoke and the biological pathways which they perturb to adversely affect the developing fetus and placenta have not been fully explained. We investigated changes in the transcriptome and methylome using RNA sequencing (RNA-Seq, n=35) and whole genome bisulfite sequencing (WGBS, n=10) on early pregnancy placenta samples with or without maternal CSE. Overall, 204 transcripts (100 up-regulated, 104 down-regulated) were differentially expressed with maternal CSE (nominal p-value <0.01). As expected, CYP1A1 expression was induced in samples with maternal CSE. Other differentially expressed genes included CGB (p<10-3) which encodes the β subunit of human chorionic gonadotropin (hCG), important for the establishment and maintenance of pregnancy. WGBS identified 458 differentially methylated regions (each containing CpGs) enriched for binding sites of transcription factors with known function in trophoblast development and response to CSE including Oct1 and AhR. Regulatory networks of the methylation signatures were obtained by applying weighted correlation matrices which identified three modules (R=0.8, p<10-3) that associated with CSE. Targeted genes mapping to these modules were identified by GREAT and pathway analysis by DAVID was applied. Strikingly, Tobacco Use Disorder (N=69 genes, p=1.16x10-5) was the top associated disease. Among the genes with altered methylation was NRG1, which promotes extravillous trophoblast formation in placental explants. In conclusion, maternal CSE alters the transcriptome and the methylome of the placenta that provides insights into the mechanisms that may lead to the increased risk of SGA of infants exposed to maternal CSE in utero. This project was funded by the Cross Foundation, Center for Pediatric Genomic Medicine Pilot Program.
-

Methods to Detect and Enrich Trimethoprim Protein Adducts in Biological Matrices
Whitney M. Nolte, Barry Preuett, and Jennifer Goldman
Background: Bactrim, the combination antibiotic trimethoprim-sulfamethoxazole (TMP-SMX), is an efficacious and broadly prescribed drug for the treatment of infections. Unfortunately, Bactrim has a high rate of idiosyncratic adverse drug reactions (IADRs), which has almost exclusively been attributed to SMX due to its well-characterized reactive metabolites and protein binding. More recent data suggests that TMP has been overlooked as a cause of these IADRs as TMP can also be bioactivated to reactive intermediates capable of reacting with thiols and potentially proteins [1]. Further studies in which radiolabeled TMP was incubated in vitro with human liver microsomes provided evidence of protein binding by TMP metabolites similar to SMX [2]. Previous in-house studies using anti-TMP antiserum detected circulating TMP protein adducts in patients taking TMP-SMX. However, methods to detect and characterize protein adducts in vivo need to be established. Here we describe the development of methods to enrich and detect TMP-protein adducts in biological matrices. Methods: To investigate whether we could detect TMP adducts in human plasma, we incubated human plasma in vitro with TMP benzylic alcohol metabolite, Cα-OH-TMP, to generate modified proteins. The samples were analyzed by western blotting and liquid chromatography-tandem mass spectrometry (LC-MS/MS) to detect and identify protein adducts. Methods to enrich TMP adducts from biological samples were also investigated. We immobilized partially purified TMP antiserum onto beads, and used these beads to enrich TMP-modified peptides from tryptic digests of HSA incubated with Cα-OH-TMP. The input, flow-through, and eluate of this enrichment were analyzed by LC-MS/MS. Results: We observed modification of plasma proteins by Cα-OH-TMP by western blotting and by LC-MS/MS. Incubation of human plasma with the Cα-OH-TMP metabolite resulted in covalent modification of HSA on the Cys34 residue. Using beads with immobilized TMP antiserum, we were able to selectively enrich TMP-modified peptides from tryptic digests of TMP-modified HSA. Conclusions: We report that Cα-OH-TMP can react with plasma proteins, and that these modified proteins can be detected by LC-MS/MS and western blotting. We also demonstrated a method to enrich TMP-modified peptides from tryptic digests. Further work is required to determine whether these methods can be applied to patient samples to detect and measure specific TMP-modified proteins in vivo. Quantification of TMP-modified proteins in vivo has the potential to yield mechanistic understanding of Bactrim IADRs and to identify prospective biomarkers of IADR development.
-

New Vaccine Surveillance Network-Acture Respiratory Infection (NVSN – ARI) Refusal Rate Analysis: Inpatient vs. Emergency Department
Anne Kleinwolterink and Rangaraj Selvarangan
Introduction: Children with acute respiratory infection (ARI) often present to hospitals. The Children’s Mercy Hospital (CM) is one of seven sites across the United States within the New Vaccine Surveillance Network (NVSN) funded by the Center for Disease Control (CDC). This network conducts active surveillance of pediatric patients who present with respiratory illness to the inpatient (IP) floors at CM and Children’s Mercy Kansas (CMK) as well as the CM Emergency Department (ED).
Method: From December 1, 2016-July 20, 2018 research coordinators screened patients at IP and ED that presented with ARI symptoms in the past 13 days, were < 18 years of age, and reside in Jackson County, Missouri. Refusals are the highest non-enrollment reason and 40%-60% of eligible patients end up not enrolling in the study. CMK/IP and ED refusals were compared by a number of variables (sex, race, ethnicity, insurance status, enrollment month, enrollment day of the week, and common symptoms).
Results:
IP enrollment vs. refusal rates for race are 49% Caucasian enroll vs. 39% refuse, 37% African Americans enroll vs. 42% refuse, 2% Multi-Racial enroll vs. 0% refuse, 2% listed other enrolled vs. 1% refuse, and 10% unknown enrolled vs. 18% refuse. ED enrolment vs. refusal rates for race are 22% Caucasian enroll vs. 14% refuse, 60% African Americans enroll vs. 50% refuse, 3% Multi-Racial enroll vs. 0% refuse, 1% listed other enrolled vs. 1% refused, and 14% unknown enrolled vs. 35% refused. In the ED more non-Hispanics enrolled (80%) than refused (64%). Families that identify as white only enroll more frequently than refuse (8-10%) for both ED and IP. The same applies for families that identify as black only in the ED (10%) difference, whereas IP has similar percentages of enrolled vs. refused for families that identify as black only. Families that identify as Non-Hispanic enroll in the ED more frequently than refuse (15%) while IP has similar percentage for ethnicity enrolled vs. refused.
Conclusion:
Sex, insurance status, enrollment month, enrollment day of the week, and common symptoms are not a significant indicator for refusal rates at IP and ED. Both race and ethnicity saw a difference between enrollment and refusals rates for IP and ED. More information is needed with the completion of S17-S18 to obtain additional data and compare findings between study seasons.
-

Psychosocial Simulation: A Novel Approach To Interprofessional Training
Barbra Rudder, Sabra Boyd, Stephanie Easley, Jill Nusbaum, Ashley K. Sherman, Dane Sommer, and Robert Schremmer
Introduction
In health care, teamwork is the foundation for efficient processes and effective outcomes and serves as a cornerstone of quality care. Good teamwork often requires training and practice. The primary aims of this study were to assess the impact of psychosocial simulations on participant knowledge of other professionals’ responsibilities and capabilities and on confidence and competence of psychosocial team members in collaborating and communicating with other psychosocial team members. Secondarily, we assessed participant satisfaction.
Methods
This single-site study used a pre- and post-survey design of social workers, chaplains, and child life specialists who attended a psychosocial simulation education module. Participants took the Psychosocial Simulation Participant Survey (PSPS), a 19-question survey tool developed by the research team. Pre- and post-simulation responses were summarized and compared using standard statistical analysis methods.
Results
Participants showed significant improvement in the subscales of Learning and Performance, Benefits of Training, and Cooperation. Two of the three Communication subscale questions showed significant improvements. Previous and current role as participant or observer, past experience with simulation, gender, discipline, age, years at institution, and area of regular assignment were not related to improvement in any of the outcomes. Over 90% of the participants agreed or strongly agreed with the statement “I was satisfied with my simulation experience” and “The post scenario discussion (debriefing) helped me to understand, reflect, and think critically.”
Conclusions
The use of simulation training with psychosocial professionals is an effective means of teaching new competencies and of promoting interprofessional collaboration.
-

Scope of Advance Practice Providers Role in Transition to Adulthood Care
Cathy Cartwright and Teresa M. Hickam
Background:
Effective pediatric transition programs are often based upon multidisciplinary teams who divide many responsibilities in teaching patients/caregivers to learn self-health management and successfully transfer to the care of an adult provider when aging out of pediatric care.
Using members of their Transition Committee, Children’s Mercy Kansas City developed a list of topics and responsibilities that could present as part of the education and services provided. As teams begin adopting transition planning practices, they are encouraged to jointly review the list and identify which team member would be responsible for addressing the item.
Methods:
The list of Transition Program responsibilities was developed into a REDCap survey. The survey also encouraged additional comments. The survey was sent electronically to the 354 advance practice nurses (APRNs) and 6 physician assistants (PA’s) employed by the hospital.
The survey asked Advance Practice Providers (APPs) to identify transition responsibilities they assume for their teams and whether other team members assume those duties in their absence. The proposal was submitted as a QI project with the hospital IRB program.
Results:
60 out of 360 APPs completed the Transition Responsibilities survey. Approximately 25% of respondents were actively using the hospital’s standardized transition planning process. The primary responsibilities generally provided only by the APP are related to medical education, follow up on test results, medication, and when to seek treatment.
Duties often delegated to the physician, staff nurse or social worker include use of patient portal, obtaining health insurance and release of information, and creating a list of providers and phone numbers.
Conclusion:
APPs are responsible for a majority of medical oversight. Further work is needed to confirm how a greater understanding of the transition planning process expands the role of the APP to include enhanced engagement with the multidisciplinary team, patient/caregiver, and transfer to adult providers.
-

Sustainability and Outcomes of a Standardized Aminoglycoside Induced Ototoxicity Monitoring Algorithm in Patients with Cystic Fibrosis
Claire Elson, Ellen Meier, and Christopher M. Oermann
Introduction: Aminoglycoside antibiotics (AG) are essential to treat infections in cystic fibrosis (CF). Potential nephrotoxicity and ototoxicity make appropriate monitoring critical. The 2016 CFF Patient Registry reports a low incidence of hearing loss (2.2% overall). However, in the United States, 13% of the total population > 12 years has hearing loss. A standardized aminoglycoside induced ototoxicity algorithm (AIOA) was implemented in 2017 at Children’s Mercy Kansas City (CMKC) to assess CF patients treated with intravenous (IV) and/or inhaled AG.
Methods: The AIOA was developed using information from CF provider surveys, retrospective chart review, observational cohort analysis, and a literature review. The algorithm is a visual reference for clinicians and provides specific AG monitoring instructions. It identifies risk factors warranting more frequent screening. The CF Center Coordinator and pharmacist are responsible for monitoring adherence to the AIOA including 1) identification of patients for monitoring during pre-clinic huddles and hospitalizations 2) review of monthly AG prescriptions, and 3) inpatient AG order review.
Results: Prior to AIOA implementation, 14 of 52 patients (27%) treated with IV AG between 2014 and 2015 hadan audiogram. Of the 70 patients that received at least two courses of inhaled AG in 2016, 18 (26%) had an audiogram. In the 24 months post-AIOA implementation, 43 of 44 patients (98%) treated with IV AG had an audiogram and of these, 27 (63%) were abnormal. Over the same period, 19 of 33 patients (58%) receiving inhaled AG for > 5 years had an audiogram completed per the AIOA. Among these, 10 (53%) were abnormal. The majority of patients (90%) received concomitant IV AG. Ten of the 30 (33%) patients that had repeated audiograms had clinically significant changes. A post-implementation provider survey demonstrated AIOA support and use of this information to influence treatment decisions. Specific interventions based on audiogram data included referral to otolaryngology for hearing aid evaluation and modifications to pulmonary exacerbation treatment regimens.
Conclusions: Implementation of an AIOA increased the frequency of audiogram screening among CF patients treated with IV and inhaled AG. The prevalence of hearing abnormalities at CMKC is higher than reported in the CFF Patient Registry and the overall US population. This discrepancy may be secondary to AG usage at CMKC or underreporting due to lack of testing. The frequent use of AG among CF patients and the probability of AG induced hearing loss suggest an urgent need to establish an AIOA nationally.
-

Use of ACTH Stimulation Test to Diagnose Adrenocortical Insufficiency in Children with Brain Tumors
Jennifer W. Boyd, Koral Shah, Kevin Ginn, Kristy Hurst, Julia Broussard, and Rakesh K. Goyal
BACKGROUND: Childhood cancer survivors with brain tumors are at high risk of developing adrenocortical insufficiency (AI).
OBJECTIVES: Primary objective of this study was to determine prevalence of AI in children with brain tumors.
DESIGN/METHODS: Under an IRB approved study, we performed retrospective chart review to identify children treated for brain tumors. Adrenocortical function was evaluated by ACTH stimulation test (“stim test”). Low-dose stim test was performed by giving 1 mcg cosyntropin intravenously and measuring serum cortisol levels at 0, 10, 20 and 30 minutes. A high-dose stim test was performed by giving 15 mcg per kg (max 250 mcg) cosyntropin and measuring serum cortisol levels at 0, 30 and 60 minutes. AI was diagnosed if peak serum cortisol levels were below 18 mcg/dL. AI was classified as (1) central AI due to direct effect on hypothalamicpituitary (HP) region by tumor, surgery, or cranial radiation therapy; (2) adrenal suppression from the effects of exogenous glucocorticoids or other medications on hypothalamic-pituitary (HP) axis; and (3) primary AI due to adrenal gland pathology.
RESULTS: Four-hundred-one children, median age 8 years (range: 0.1 – 19) were diagnosed with brain tumors between 2006-2017 at our institution. Adrenocortical function testing was performed on 56 patients. A total of 72 stim tests were performed, and no adverse effects were noted. Of these 52 were high-dose, 13 were low-dose, and 7 were low-dose followed by highdose. AI was observed in 16/56 (29%) cases. All cases (16/16, 100%) were considered to be central, related to direct tumor effects on HP region, cranioradiation therapy and / or surgery. Exogenous glucocorticoids or megestrol causing adrenal suppression contributed in 4 (25%) cases. Amongst those undergoing stim testing, other endocrinopathies were common (43/56, 77%). We observed a higher rate of AI in patients with direct involvement of HPA by tumor (41% vs. 21%), and those undergoing surgery in HPA region (63% vs. 21%), and those with other endocrinopathies (33% vs. 18%).
CONCLUSIONS: We observed a high prevalence of AI in pediatric patients with brain tumors. Children with tumors involving the HP region are at high-risk and should have adrenal function evaluated early especially prior to intracranial surgery. Children with medulloblastomas who received cranial radiotherapy, and those with multiple endocrinopathies should be screened for late onset central AI. ACTH stim test is a useful and objective measure of hypothalamicpituitary- adrenal axis function and should be considered in routine practice in management of this high-risk population.
-

Use of ACTH Stimulation Test to Diagnose Adrenocortical Insufficiency in Pediatric HCT Recipients
Koral Shah, Rakesh Goyal, Rukhsana Rahmetulla, and Julia Broussard
BACKGROUND: Children undergoing hematopoietic cell transplantation (HCT) are at high-risk of developing adrenocortical insufficiency (AI).
OBJECTIVES: Primary objective of this study was to determine prevalence of AI in pediatric HCT recipients.
DESIGN/METHODS: Under an IRB approved study, we identified HCT recipients who were tested for AI at our institution. Adrenocortical function was evaluated by ACTH stimulation tests (stim test). A low-dose stim test was performed by giving 1 mcg cosyntropin intravenously and measuring serum cortisol levels at 0, 10, 20 and 30 minutes. A high-dose stim test was performed by giving 15 mcg per kg (max 250 mcg) cosyntropin and measuring serum cortisol levels at 0, 30 and 60 minutes. AI was diagnosed if peak serum cortisol level was below 18 mcg/dL. AI was classified as (1) adrenal suppression from the effects of exogenous glucocorticoids or other medications on hypothalamic-pituitary (HP) axis, (2) central AI due to direct effect on HP region by tumor, surgery, or cranial radiation therapy; or (3) primary AI due to adrenal gland pathology.
RESULTS: Between years 2006 -2017, 269 patients, median age 10.2 years (range 0.1 – 22.4) underwent 349 transplants (59% allogeneic, 41% autologous). Of these, 66 patients who had 87 transplants underwent adrenocortical function testing. In those tested, a majority of the transplants were allogeneic (73.6%) and were performed for malignant diseases (66.7%); and 38 patients had prior glucocorticoid exposure (57.6%). A total of 83 stim tests were performed, and no adverse effects were noted. Of these, 63 were high-dose, 6 were low-dose, and 14 were low-dose followed by high-dose. AI was observed in 14/66 patients (21%). The most common cause of AI was adrenal suppression (12/14 cases, 86%); 10 had exposure to glucocorticoids and 2 to megestrol. One patient had primary AI related to MIRAGE syndrome, and another from adrenal gland resection. There was a higher rate of AI in patients with acute GVHD (29%) compared to those without acute GVHD (12%). Of the 31 children with acute GVHD, 23 (74%) were found to have normal adrenal gland function despite prior glucocorticoid exposure.
CONCLUSIONS: We observed a high prevalence of AI in pediatric HCT recipients. The stim tests demonstrated recovery of HPA axis in a majority of patients with acute GVHD and prior glucocorticoid exposure. ACTH stimulation testing is a useful, objective measure of HPA axis function; it should be used to guide replacement and stress dosing of glucocorticoids in high risk HCT recipients.
-

Worldwide Experience with Peritonitis in Children: A Report from the International Pediatric Peritoneal Dialysis Network (IPPN)
Bradley Warady, Dagmara Borzych-Duzalka, and Franz Schaefer
Background:
Peritonitis is a significant risk factor for peritoneal dialysis (PD) technique failure in children receiving chronic PD. The IPPN is the only source of pediatric PD infection related data obtained on a global basis.
Objective:
To describe the peritonitis rate, etiology, antibiotic susceptibility, clinical presentation and outcome experienced by patients whose data was entered into the IPPN registry.
Methods:
Review of prospectively collected data submitted to the IPPN registry via an Internet-based web platform (www.pedpd.org) between 2007-2015. Data pertaining to patient characteristics, dialysis modality, microbiological results, and final outcome were submitted prospectively along the course of a peritonitis episode. The statistics were performed by univariate and multivariable logistic regression analysis.
Results:
Data from 3,162 patients in 43 countries was entered into the registry. The highest percentage of patients came from Western Europe (24%) and Asia/ME (23%). Sixty-six % of the patient were < 12 years of age and automated PD was the predominant PD modality. Overall, there were 2021 episodes of peritonitis reported in 1052 patients with an annualized peritonitis rate of 0.44. The annualized rate varied by region (p=0.01) with the lowest rates present in Asia/ME (0.3) and North America (0.38). Risk factors for peritonitis included use of CAPD vs. APD (OR 1.13, p=0.01), upward pointing exit site (OR 1.26, P < 0.001) and presence of any ostomy (OR=1.95, p < 0.001), Clinical symptomatology was greatest with gram negative associated episodes (p < 0.001). S. Aureus and S. Epidermidis were the most frequently isolated organisms and culture negative peritonitis was most common in Turkey and Latin America. Significant regional variation in antibiotic susceptibility was noted for aminoglycosides and methicillin. Full functional recovery occurred in 82% of cases, with no regional variation. 175 patients (8.7%) permanently discontinued PD following peritonitis.-
Conclusion:
Peritonitis remains a frequent complication associated with the performance of PD in children. Attention to risk factors for infection may help decrease the regional variation present in the rate of peritonitis. Risk factors for culture negative peritonitis in specific global regions should continue to be sought.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.



