Publication Date
3-2021
Files
Download Full Text (281 KB)
Abstract
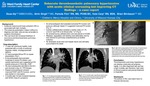
ackground: • Subacute massive pulmonary embolism (PE) is associated with high mortality. • The subacute presentation makes it difficult to diagnose and older clots are less amenable to systemic thrombolysis. • This can result into increased likelihood of recurrence and thromboembolic pulmonary hypertension Case description: • 17-year-old, previously healthy male presented with a month of exertional dyspnea, initially misdiagnosed with asthma. • CT demonstrated diffuse PE on repeat presentation (Fig1). • Echocardiography demonstrated moderate to severe RV dilation and systolic dysfunction and suggested an RV systolic pressure of 73mmHg + RAP. • He was subsequently admitted to the ICU and received a day of r-TPA therapy. • Repeat echocardiogram showed improved RVSP and RV function, and he was started on rivaroxaban. • 3 months later he had increased dyspnea with NYHA Class III symptoms • An echocardiogram demonstrated worsened RV function and pressure, although repeat CT suggested improved PE burden (Fig. 2). • Cardiac catheterization revealed a cardiac index of 1.75 L/min/m2 and PVR of 23 Wood Units * m2 (Fig 3). • He arrested during catheterization and was placed on ECMO. • Alteplase, angioplasty and stenting were attempted, and he was referred for pulmonary endarterectomy at another institution. • He developed acute renal and hepatic failure and ultimately succumbed to his death. Conclusion: Thromboembolic pulmonary hypertension can develop subacutely yet progress rapidly. It is often diagnosed late and has a high mortality rate; therefore, high index of clinical suspicion and prompt treatment is imperative. Disclosure: The authors of this case report have no financial disclosures. Fig 1: CT at initial presentation demonstrating widespread PE with multiple filling defects seen throughout the segmental pulmonary arteries to all lobes of both lungs Fig 2: CT 3 months later, significant obstruction of the distal pulmonary vasculature bilaterally and pruning, giving a false impression of improved clot burden Fig 3: (a) Cath angiography on the first day of readmission (3 month post initial presentation, showing significant obstruction of the right lobar arteries and severely attenuated peripheral pulmonary vasculature. (b) cath angiography on the following day showing rapid progression with almost absent peripheral vascular flow.
Disciplines
Cardiology
Recommended Citation
Aly, Doaa; Singh, Alvin; Finn, Pamela; Carp, Kate; and Birnbaum, Brian, "Subacute thromboembolic pulmonary hypertension with acute clinical worsening but improving CT findings - a case reporrt" (2021). Posters. 231.
https://scholarlyexchange.childrensmercy.org/posters/231




Notes
Presented at the 14th International Symposium on Neonatal and Childhood Pulmonary Vascular Disease Conference; March 3 - 5, 2021; Virtual conference- UCSF San Francisco.