Publication Date
12-2021
Files
Download Full Text (1.2 MB)
Abstract
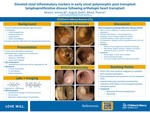
Acute gastrointestinal hemorrhage in the context of a recent organ transplant with immunosuppression, antibiotic exposure, drug exposures and other comorbidities is a challenging clinical scenario with coordinated multidisciplinary effort needed to optimize management and outcomes. We present a patient with recent solid organ transplant with severe acute gastrointestinal bleeding attributable to EBV associated post-transplant lymphoproliferative disease. The patient is a 13-year-old Female with Williams syndrome who is EBV negative and CMV positive who received an EBV/CMV positive orthotopic heart transplant 5.5 months prior to presentation. She presented with bloody diarrhea, anemia (7.8 gm/dL), hypovolemia, and acute kidney injury (BUN 25 mg/dL - baseline 8-12) and admitted for IV fluid replacement, blood transfusion, and IV Iron infusion. Fecal calprotectin was 938 mcg/g and stool lactoferrin was 379.8 mcg/mL. MR enterography demonstrated inflammatory changes of the terminal ileum without evidence of stricture and prominent (reactive) mesenteric lymph nodes. EGD and Colonoscopy on day 8 of admission revealed multiple, sessile, semi-pedunculated, moderately vascular and raised lesions with central umbilication and granulation tissue at the apex ranging in size from 0.3 to 1 cm in the stomach, duodenum, terminal ileum, and the colon with similar findings in the small bowel on capsule endoscopy. She also had esophagitis, non-specific mild, chronic gastritis, normal terminal ileal and colonic mucosal biopsies with no inflammatory changes. Margin biopsies were infiltrated with a variable lymphoid cell population throughout the lamina propria, glandular architectural distortion, and focal gland destruction. The lymphoid cells were variable in size with small (CD3/CD43 positive) and large (CD20/CD43 positive) lymphocytes with vesicular chromatin and occasional prominent nuclei. EBER CISH was positive in many of the abnormal cells. She was diagnosed with EBV positive, polymorphic post-transplant lymphoproliferative disease (PTLD). Following a pre-treatment PET/CT scan revealing abnormal activity throughout the neck, chest, abdomen, and pelvis, she was started on rituximab, maintained tacrolimus with a goal serum level of 5-10, whereas MMF was withheld. PTLD is caused by proliferation of lymphoid or plasma cells and is the most common malignancy in the pediatric transplant population. The hallmark is EBV infection in the context of immunosuppression, occurs in approximately 2-15% of organ transplant recipients, can present with fever, lethargy, weight loss, generalized malaise, and lymphadenopathy but may also present with symptoms specific to the organ affected. Outside the gastrointestinal tract, PTLD can develop in the lymph system, central nervous system, lung, and liver. Gastrointestinal involvement includes bleeding, anemia, hypoalbuminemia, protein-losing enteropathy, and diarrhea. Treatment includes reduction in immunosuppression followed by a chemotherapeutic agent such as rituximab. Treatment can also involve surgical resection, radiation, anti-CD20 antibody therapy, or cytotoxic T-cell therapy. Outcomes vary by transplanted organ and can result in organ failure secondary to rejection and even death but with higher overall survival rates in children. The case presented is interesting insofar as the early presentation is atypical and it also illustrates the elevation in stool inflammatory markers, both lactoferrin and calprotectin, which has not previously been reported in the literature. The elevated stool markers are also interesting given the lack of gross morphologic or biopsy proven inflammation in non-lesion pathology. Our report underscores the utility of stool inflammatory markers in gastrointestinal bleeding in the solid-organ transplant recipient.
Disciplines
Gastroenterology
Recommended Citation
Stewart, Jeremy; August, Keith; and Attard, Thomas M., "Elevated stool inflammatory markers in early onset polymorphic post-transplant lymphoproliferative disease following orthotopic heart transplant" (2021). Posters. 247.
https://scholarlyexchange.childrensmercy.org/posters/247




Notes
Presented at the Virtual NASPGHAN (North American Society for Pediatric Gastroenterology, Hepatology & Nutrition) Annual Meeting, Postgraduate Course and Single Topic Symposium were held live December 12-18, 2021