-

Acceptability And Behavior Change In A Pilot mHealth Physical Activity Intervention
Mallory Moon, Chelsea Steel, Cory Yeager, Kacee Ross, Frank T. Materia, Delwyn Catley, Harpreet Gill, Jannette Berkley-Patton, Karynn E. Glover, and Jordan A. Carlson
Background and Purpose.
Increasing resources for meeting physical activity guidelines is important for reducing health disparities experienced in marginalized communities. Mobile health (mHealth) interventions are particularly promising for delivering low cost, wide reaching interventions, but few interventions exist that are appropriate for youth and adults from this population group. This study evaluated a pilot mHealth physical activity intervention, Active KC, delivered to children and adults from marginalized communities in Kansas City, MO.
Methods.
164 participants aged 8-88 years (83% Black, 81% female) recruited through community health events and Children’s Mercy primary care clinics were enrolled into Active KC. The 7-week theory-based intervention followed a 1-week baseline and integrated a Garmin activity monitor with personalized text messages sent by an automated system developed by Children’s Mercy Research Institute’s Research Informatics team. Messages were sent 5 days each week to facilitate self-monitoring and self-efficacy based on the participant’s Garmin health data. Post-intervention surveys were used to measure intervention acceptability. Garmin data were analyzed using mixed-effects regression to evaluate changes in daily step counts.
Results.
A priori analytic inclusion criteria resulted in an analytic sample of 29 youth and 66 adults (≥1 day of baseline data and <40 and><20 minutes>/day of MVPA at baseline, respectively). Youth’s daily steps increased from a mean of 6,356 (SD=2,040) at baseline to 7,056 (SD=2340) at Weeks 6-7 (B=700, 95% CI=-644, 2045, ES=0.34). Adult’s daily steps increased from a mean of 4,124 (SD=1,447) at baseline to 4,697 (SD=1,931) at Weeks 6-7 (B=573, 95% CI=-65, 1211, ES=0.40). Daily step increases were larger in those with lower baseline values (increases of B=1795 and B=1724 for youth and adults) and who engaged more with the text messages (B=1,011 and B=903). 99% of participants indicated the intervention helped them be more physically active and 98% indicated they would recommend the intervention to family and friends. Qualitative data indicated that parents and children particularly enjoyed participating in the intervention together. Participants provided input on content appropriateness and refinements while and after receiving the intervention.
Conclusions.
Results indicate mHealth interventions that integrate consumer wearables and personalized text messaging can have high acceptability and support increases in physical activity in a marginalized community sample. Future research will focus on enhancing implementation and evaluating optimal levels of resources and contact necessary for improving participant adoption, engagement, and intervention effectiveness.
-

A genomics driven pluripotent stem cell model of infant acute lymphoblastic leukemia
Jacqelyn Nemechek, Julia Draper, Sarah McDermott, Irina Pushel, Midhat S. Farooqi, Erin M. Guest, John M. Perry, and Jay L. Vivian
Acute lymphoblastic leukemia in infants (iALL) is a high-risk subtype of childhood leukemia, with poor survival outcomes despite intensive therapies. Rearrangement of KMT2A (KMT2A-r) on chromosome 11q23 is the most frequent cytogenetic abnormality in both iALL and pediatric acute myeloid leukemia (AML). Survival outcomes for children with KMT2A-r leukemia are generally very poor, despite intensive therapies, as KMT2A-r is associated with refractoriness to therapy and early relapse. KMT2A-r generates a driver fusion oncogene, most commonly KMT2A::AFF1 or KMT2A::MLLT1 in ALL, and KMT2A::MLLT3 in AML, resulting in epigenetic dysregulation of target gene transcription. iALL expressing MLL-AF4 is an unusual cancer in that other somatic mutations are uncommon and there are no known genetic risk factors. Our team has discovered rare pathogenic genomic variants in healthy blood cells from infants in remission from ALL. We detected germline variants in ERCC2 and MITF in multiple cases of MLL-AF4 ALL, and these were validated using external databases. We hypothesize that these and perhaps other rare, pathogenic variants detected in cancer predisposition genes impact the onset, severity, and response to therapies in KMT2A-r ALL. Unfortunately, research into this rare but devasting disease has been hindered by a lack of appropriate, representative models. This indicates an essential, outstanding need for the development of more representative model systems for KMT2A-r leukemias. Interestingly, iALL originates in utero with the most aggressive cases being associated with an early embryonic or fetal origin; however, little is known regarding how KMT2A-r subverts early hematopoiesis, the cell types of origin, or how it controls progression to leukemia.
In an effort to understand the role of newly discovered germline variants associated with iALL, we have created a highly controlled induced pluripotent stem (iPS) cell model system to understand the genomic and epigenetic landscape of iALL. Specifically, we engineered human iPS cell lines to express MLL-Af4 fusion and are employing CRISPR gene editing technology to introduce clinically identified variants of interest. Furthermore, we have used directed differentiation to produce functional human hematopoietic stem and progenitor (HSPCs) from iPS cells. Notably, this model recapitulates hematopoietic ontogeny. Our iPS cell-based iALL cell model system provides the opportunity to investigate a range of critical and outstanding questions of iALL disease initiation, progression, and treatment. Future studies include a comparison of this model to single cell transcriptomic datasets from pediatric leukemia patients from our Cancer Center Biorepository, and comparison with developmental datasets from human embryonic and fetal hematopoiesis.
-

A novel and comprehensive testing strategy to identify the genetic etiology of neonatal hypotonia phenotypes
Jasmine A. McQuerry, Margaret Gibson, Scott T. Younger, T Pastinen, and Emily G. Farrow
Neonatal hypotonia (NH) is a common, non-specific symptom manifested in numerous and disparate disorders of genetic origin. These disorders can be caused by diverse genetic changes including chromosomal aberrations, copy number variations (CNVs), methylation changes, trinucleotide repeat expansions, and single nucleotide variants (SNVs). Currently, no single laboratory testing modality is available to test these disparate etiologies. We have designed a targeted sequencing approach to identify and prioritize genetic changes in loci related to NH phenotypes in a single test, thus reducing the number and types of tests required to make a diagnosis. This amplification-free approach uses CRISPR/Cas9 DNA cutting technology to produce targeted sequencing libraries of NH related genomic loci for sequencing using the PacBio Sequel IIe system, which sequences native DNA in long reads, allowing for the detection of methylation changes, trinucleotide repeat expansions and CNVs that can be missed by typical short read sequencing. We designed a set of guide RNAs (gRNAs) targeting a panel of 116 NH loci of interest. To maximize Cas9 cutting at each locus, gRNAs were chosen such that 3 gRNAs cut upstream and 3 downstream of each target. Size-based sequencing bias was avoided by constraining all target loci to 11-14 kilobases in length; thus, most genic loci required division into multiple fragments for sequencing, for a total of 1050 fragments in the panel. We in vitro transcribed the resulting library of 6300 guide RNAs (1050 fragments x 6 gRNAs) from DNA oligonucleotides. Remarkably, when complexed with Cas9, this highly multiplexed gRNA library successfully cut NH loci from patient genomic DNA isolated from blood as evidenced by the inability to produce polymerase chain reaction amplicons across the targeted Cas9 cutting sites. Additionally, no off-target cutting was identified at several nearby regions tested. This specific cutting allows for production of targeted sequencing libraries of native DNA containing only the NH loci of interest. We anticipate that optimization of this method will reduce costs and turnaround time for hypotonia diagnoses in the future. Additionally, this approach can be applied for testing in other complex disorders, or to produce any targeted sequencing panel containing native genomic regions of interest in a cost-effective and multiplexed manner.
-

A Pilot Study of Azacitidine as Epigenetic Priming for Chemotherapy in Infants Less Than 1 Year of Age with KMT2A-Rearranged Acute Lymphoblastic Leukemia (ALL); Results from the Children’s Oncology Group (COG) Trial AALL15P1
Erin M. Guest, John Kairalla, Meenakshi Devidas, Emily Hibbitts, Andrew Carroll, Nyla A. Heerema, Holly Kubaney, Amanda August, Melinda Pauly, Daniel Wechsler, Rodney Miles, Joel Reid, Cynthia Kihei, Lia Gore, Elizabeth Raetz, Stephen Hunger, Mignon Loh, and Patrick Brown
Introduction
Acute lymphoblastic leukemia (ALL) with KMT2A-rerrangement (KMT2A-r) in infants < 1 year is a high-risk childhood ALL subtype, with consistently poor event-free survival (EFS) of approximately 35% when treated with intensive chemotherapy with or without hematopoietic stem cell transplant. Infant ALL blasts are characterized by DNA hypermethylation, which is hypothesized to contribute to chemoresistance by altering transcriptional regulation of gene expression. In preclinical studies of KMT2A-r blasts, epigenetic priming with DNA methyltransferase inhibitors improved the in vitro cytotoxicity of chemotherapy. Azacitidine, a pyrimidine nucleoside analog of cytidine and hypomethylating agent, has been used in combination with chemotherapy in children with leukemia. We previously reported that azacitidine was safe and well tolerated in AALL15P1 (ASPHO 2021) and herein we report survival outcomes.
Methods
The Children’s Oncology Group (COG) trial AALL15P1 (NCT02828358) was a single arm, open label, groupwide pilot trial. The primary aim of the trial was to evaluate the tolerability of azacitidine in addition to Interfant-06 standard chemotherapy in infants with newly diagnosed KMT2A-r ALL. Estimation of 5-year EFS was an exploratory aim, given the small sample size. Eligibility criteria included B-ALL or acute leukemia of ambiguous lineage with ≥50% B-lymphoblasts, <366 days of age at>diagnosis, and >36 weeks gestational age at enrollment. Exclusions included Down syndrome, secondary ALL, and prior cytotoxic therapy (except intrathecal chemotherapy or corticosteroids). Following an Interfant-based induction, infants with KMT2A-r received 4 courses of azacitidine, 2.5 mg/kg/dose intravenously over 10-40 minutes daily for 5 consecutive days in each course, immediately preceding the start of a chemotherapy course on day 6. Infants without KMT2A-r were removed from protocol following induction and did not receive azacitidine. Treatment failure was defined as failure to achieve M1 marrow status (< 5% blasts by morphology) with resolution of extramedullary leukemia by the end of consolidation. EFS and overall survival (OS) were measured from the time of enrollment.
Results
The study accrued from March 2017 to December 2019 and all protocol-directed treatment concluded in December 2021. Of the 78 infants enrolled, 56 had KMT2A-r (72%), and 53 completed induction therapy and received at least 1 course of azacitidine. No patients were ineligible. Diagnostic clinical characteristics of infants with KMT2A-r included four infants age <7 days>(7%), 13 age <90 days>(23%), 18 with white blood cell count ≥300,000/μL (32%), 32 CNS2 (57%), and four CNS3 (7%). As of the data cutoff (06/30/2022), the median follow-up is 3.8 years, and the 3-year EFS (SE) and OS (SE) rates are 34.2% (+/- 0.08) and 63.8% (+/-0.08), respectively, for infants with KMT2A-r. Six infants experienced treatment failure. Minimal residual disease (MRD) levels of marrow blasts by flow cytometry in COG-approved laboratories were submitted for 49 KMT2A-r patients at the end of induction. Of those, 32 were MRD negative <0.01% (65%), eight MRD positive 0.01%-<1% (16%) and nine MRD positive ≥1% (18%). Event-free survival was significantly associated with MRD; the 3-year EFS of patients with any positive MRD was 20.6% (+/-0.13) vs. 40.1% (+/-0.09) (p=0.0185) for those without MRD. As previously reported, at no time did the trial meet or exceed the pre-determined dose limiting toxicity boundaries, and the rates and types of toxicities observed were within the expected range for infants receiving standard chemotherapy alone. Conclusions
Epigenetic priming with azacitidine prior to standard chemotherapy was well tolerated in infants with KMT2A-r ALL, but the EFS was consistent with the poor survival of historical outcomes. Positive flow MRD at the end of induction predicted a higher risk of treatment failure in comparison to negative MRD, but EFS was still unacceptably low for MRD-negative
-
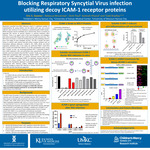
Blocking Respiratory Syncytial Virus infection utilizing decoy cell surface receptor proteins
Eric S. Geanes, Rebecca McLennan, Oishi Paul, Santosh Khanal, and Todd Bradley
Respiratory syncytial virus (RSV) infections result in a significant number of hospitalizations for young children and the elderly each year, and current infection rates continue to rise, leading to a substantial public health burden. While numerous vaccine candidates are in clinical trials, there is currently no approved RSV vaccine to prevent infection or antiviral treatment after infection. There is an urgent need to find new therapeutics and strategies that reduce severe RSV disease that could improve health and save lives. The RSV fusion (F) protein is critical for binding host cells and mediating infection and is the target of most candidate vaccines. The RSV F protein has been shown to interact with several host-cell surface receptor proteins and infect respiratory epithelial cells. In this study, we confirmed several selected cell surface receptors could bind RSV F protein and inhibit RSV infection via an RSV neutralization assay. Using RSV F protein as bait, we immunoprecipitated RSV F interacting proteins from A549 respiratory cells and performed mass spectrometry analysis to identify novel host proteins that bind RSV F protein. Finally, we engineered a mRNA-lipid nanoparticle (LNP) expressing soluble cell surface receptors. The goal is to utilize the surface receptor mRNA-LNP as a passive intranasal vaccine that would result in over-expressed soluble receptors in respiratory mucosal surfaces to function as decoy receptors that would reduce RSV infection. We are evaluating this therapeutic approach in preclinical models as a prophylactic or treatment after infection. Respiratory tract cell surface receptor mRNA-LNPs may provide a novel defensive strategy to reduce RSV infection or disease severity and augment future RSV vaccines that become approved.
-
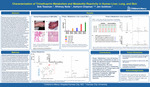
Characterization of Trimethoprim Metabolism and Metabolite Reactivity in Human Liver, Lung, and Skin
Robert T. Tessman, Whitney M. Nolte, Ashlynn Chipman, and Jennifer Goldman
Idiosyncratic adverse drug reactions (IADRs) occur in a small but significant percentage of the population, are unpredictable, and frequently cause life-threatening events requiring intensive medical care. The antibiotic, trimethoprim-sulfamethoxazole (TMP-SMX) is generally considered a safe and effective drug but has a relatively high rate of IADRs. Through metabolism, drugs may be bioactivated, yielding reactive metabolites which covalently bind to proteins making them a target for immune-mediated responses, and in some cases, fulminant drug hypersensitivity. Although the liver is the dominant contributor to drug metabolism, other organ systems are known to be metabolically active. Interestingly, TMP-SMX IADRs are associated with serious lung injury and/or mild to serious skin rash. Historically, SMX has been suspected of being the source of IADRs associated with TMP-SMX due to the formation of a reactive nitroso intermediate but more recent studies indicate that incidences of IADRs in the case of TMP use alone are higher than the combination drug, suggesting that SMX is not the sole cause of TMP-SMX IADRs. In this study, we seek to evaluate TMP metabolism in lung and skin and to assess the reactivity of any metabolites formed. Ex vivo subcellular s9 fractions contain active drug metabolizing enzymes and with the addition of appropriate co-factors, both phase I and II metabolites can be produced in vitro. Using this system, we discovered differential TMP metabolism in lung and skin as compared to liver. Liver, lung, and skin s9 reaction products were analyzed by liquid chromatography/mass spectrometry (LC/MS) Waters triple quadrupole instrument. The reactivity of tissue-specific metabolites was assessed by adding glutathione, n-acetyl cysteine, and n-acetyl lysine to s9/TMP reaction products (trapping assays). Trapping assay products were analyzed using a high-resolution Waters quadrupole/time of flight (qTOF) mass spectrometer. Results of this analysis were fed into a pick-picking algorithm (XCMS) to identify unique features against several negative controls. Using these approaches, we observed glucuronide conjugate formation in lung and sulfate conjugation in skin. Along with this novel discovery, we identified 2 potentially reactive sulfate conjugates of 4-desmethyl trimethoprim. These findings indicate that primary metabolites formed in the liver can undergo further bioactivation in lung and skin, the sites of clinical presentation of TMP IADRs. These findings are key mechanistic insights and will advance efforts to understand the etiology of this currently idiopathic medical condition.
-

Characterizing goal setting by the Registered Dietician for adolescents with newly diagnosed Polycystic Ovary Syndrome (PCOS)
Manasa Gadiraju, EM Green, Tania S. Burgert, A MacMillan Uribe, and Heidi Vanden Brink
-

Ciclesonide protects against LPS-induced lung endothelial inflammation and acute lung injury
Heather Menden, Sherry M. Mabry, and Venkatesh Sampath
Background: Synthetic glucocorticoids (sGC) are used to prevent bronchopulmonary dysplasia (BPD) in preterm infants. Ciclesonide (CIC), a sGC pro-drug, is FDA-approved for treatment of children with asthma. We reported that in comparison with dexamethasone, CIC does not affect brain development when used in the neonatal period. We have also shown that LPS, derived from gram negative bacteria, causes lung endothelial cell (EC) immune activation that contributes to sepsis-induced acute lung injury (ALI). In this study, we hypothesized that LPS-induced endothelial inflammation and ALI will be inhibited by CIC.
Objectives: a) Investigate the mechanisms by which CIC inhibits lung EC inflammation and injury, and b) Test whether CIC can repress systemic LPS-induced acute inflammation in neonatal mice.
Methods: Primary human pulmonary microvascular endothelial cells (HPMEC, ScienCell) incubated with 0.1uM CIC for 6hrs followed by treatment with 100ng/mL LPS were used to measure inflammation by western blotting, 2D angiogenesis, and qRT-PCR. Neonatal mice were i.p injected with 2mg/kg LPS, with subsequent i.p CIC (2.5mg/kg) injections at +2- and +26hrs. At 48hrs post LPS injection, bronchoalveolar lavage (BAL) was done to probe inflammatory cell influx and alveolar edema.
Results: CIC-induced expression of CES1 and CES2, enzymes that convert CIC to its active metabolite des-CIC, as well as the glucocorticoid receptor (GR) target genes FAM107A and FKBP5 (Fig. 1A-B) in HPMEC. LPS-induced expression of ICAM1, IL1β, and iNOS was suppressed by CIC (Fig. 1C-D). LPS-induced Toll Like receptor 4 signaling evidenced by (p)IKKβ and (p)p65 was attenuated by CIC (Fig. 1E). Cell viability decreased with LPS and was restored with CIC (Fig. 2A). LPS-induced VEGF and delta like 4 (regulators of angiogenesis) expression and aberrant 2D angiogenesis in HPMEC were suppressed by CIC (Figs. 2B-E). In our neonatal sepsis mouse model, CIC attenuated the influx of immune cells and vascular leakage seen 48hrs after LPS in the lung (Fig. 3A-B).
Conclusions: CIC protects against LPS-induced inflammation and EC injury in HPMEC. Sepsis (LPS)-induced lung inflammatory cell influx and vascular permeability was inhibited by CIC in our neonatal mice. Further animal studies will determine whether sepsis-induced neonatal ALI and alveolar remodeling is mitigated by CIC.
-

Detection of Enterovirus D68 in Samples Enrolled in the New Vaccine Surveillance Network from January to December 2022
Amanda Hayes, Dithi Banerjee, Anjana Sasidharan, Minati Dhar, Gina Weddle, Kirsten Weltmer, Jennifer E. Schuster, Mary Moffatt, and Rangaraj Selvarangan
Background: In 2014, the largest cohort of pediatric EV-D68 disease in the U.S. was reported by a large mid-west free-standing children’s hospital. Shortly after, reports of increased EV-D68 around the world were announced. Since then, EV-D68 has circulated even years during the summer to fall months. In June 2022, an increase in Rhinovirus/Enterovirus (RV/EV) infections with symptoms resembling EV-D68 outbreaks were noted earlier than usual in Kansas City’s clinical setting. Common symptoms of EV-D68 infection resemble asthma and severe EV-D68 infection has been linked to those with a history of asthma. Our aim was to investigate the rate of EV-D68 infections in children enrolled in the Center of Disease Control and Prevention (CDC)’s New Vaccine Surveillance Network (NVSN) acute respiratory infections (ARI) study.
Methods: Between January-December 2022, children < 18 years old seen at the hospital with symptoms of respiratory infection were enrolled into the CDC’s NVSN ARI study. Nasal samples collected in universal transport media were tested by NxTAG® Respiratory Pathogen Panel (Luminex) multiplex assay that can simultaneously detect 20 respiratory pathogens. Those with RV/EV detections were further tested by a real-time EV-D68 RT-PCR. Demographic and clinical information were also collected throughout the season.
Results: A total of 2,514 samples were tested; RV/EV was detected in 27% (n=690). EV-D68 was detected in 13.5% (n=93/690) of positive RV/EV samples, with an overall 3.7% (n=93/2514) rate of EV-D68 detection. EV-D68 was found highest in Black/African Americans (50%); in children ages 1-4 years (66%) and in males (57%). EV-D68 was more prevalent in subjects enrolled in the emergency department setting (57%) compared to the inpatient (30%) and clinic settings (13%). The most common symptoms reported by subjects and their families were coughing (97%), nasal congestion (90%), and rapid shallow breathing (77%). All 93 EV-D68 positives were detected in the summer to fall months (June to September).
Conclusions: The detection of EV-D68 within the CDC’s surveillance network brought an early awareness to the symptoms and diagnosis of this illness. These findings were reported to the CDC and in September 2022, a health advisory stating the increase in EV-D68 prevalence in hospitals and clinics nationwide was reported. Data gathered and presented here can contribute to early detection and preparedness for future outbreaks.
-

Early milk feeding impacts health and immunity in later life
Rebecca McLennan, Eric S. Geanes, Angela Dickerson, and Todd Bradley
Infants born premature have increased susceptibility to infection and other immune complications. Human milk feeding has been associated with fewer infections and reduced intestinal inflammation leading to improved health outcomes. The composition of milk is variable between mothers and changes over the course of lactation to meet the needs of the growing infant. There is an urgent need to define the components of milk that are critical for protecting against infection and improving infant health. Premature infants often receive combinations of feeding that includes donor milk that is derived from mature milk. Thus, premature infants could receive milk that lacks critical components present in early milk or colostrum. In this study, we determined the impact of early colostrum feeding had on long term health outcomes using a mouse cross-fostering feeding model. We compared body weight, fat composition, and antibody responses to Respiratory Syncytial Virus (RSV) vaccine over time in pups who were fed limited, normal, or excess amounts of colostrum. These conditions were achieved by cross fostering newborn and 1 week old mouse pups. We found that pups who ingested limited colostrum had a reduction in body weight compared to pups that ingested normal amounts of colostrum. Furthermore, this weigh discrepancy was maintained for at least the first month of life, corresponding to the juvenile stage of development. There were also differences in the antibody response to the RSV vaccine in the pups that did not receive colostrum. These experiments will provide key insights into the importance of colostrum and milk derived-immune factors on infant development.
-

Exploring Pediatric Cardiac Readmissions in the Interstage Period Using the CHAMP Multi-Site Repository
Ryan Thompson, Amy Ricketts, Janelle R. Noel-Macdonnell PhD, Keith Feldman, and Lori A. Erickson
Background: Infants with congenital heart disease (CHD) require continued and complex care in the first year of life, including regularly scheduled clinic visits. Unfortunately, given the high-risk nature of these patients, care also frequently includes hospital readmission which contributes to a high level of burden on the health care system, patient, and family who often live far from treatment centers. Remote home monitoring has successfully reduced unplanned readmissions and intensive care days during readmissions. We aimed to explore the readmissions that are occurring after the neonatal hospital discharge through the end of remote home monitoring through the interstage period using a multi-site cardiac registry.
Methods: Retrospective descriptive analysis of data from the 12 US pediatric cardiac hospitals participating in the Children’s High Acuity Monitoring Program (CHAMP®) Cardiac Research Repository between 2014-2022 (90.5% of patients).CHAMP® is a remote patient monitoring mobile application developed at Children’s Mercy utilized to enable the asynchronous transfer of remote home monitoring data. Demographics and data evaluated included length of stay (LOS), unplanned cardiac procedures, and red flag concern events through the interstage.
Results: Across n=999 subjects, most infants were term, white (79.9%), non-Hispanic (84.0%), male (62.2%), and non-syndromic (79.3%) with CHD being their only congenital anomaly (80.4% with no other major anomaly). Mothers of infants primarily spoke English (92.5%), with 48% being 26 years of age or less, and treating pediatric cardiac hospitals. Of the CHAMP®-monitored infants, 1,944 total interstage readmissions were recorded with a mean of 3 per infant across all sites. Median (IQR) time from neonatal discharge to first readmission was 62.0 (27.0-102.0) days. Median (IQR) LOS during readmissions was 3.0 (1.0-9.0) days with 43.4% of readmissions having ICU days at a median LOS 2.0 (1.0-8.0) days. In total, 576 (29.63%) included unplanned cardiac reinterventions.
Conclusion: The CHAMP cardiac multi-site registry provides insights into a relatively rare CHD at a single-site level but is robust with a multi-site repository. A well-represented infant cohort had an average of three interstage readmissions per infant occurred across all 12 hospitals. First readmissions occurred about 2 months from the neonatal discharge, LOS around a week with numerous ICU days and 30% requiring an unplanned cardiac reintervention. This understanding of interstage readmissions is key to beginning an in-depth analysis of readmission patterns by reason for admission and remote monitoring concerns prompting readmission.
-

High-throughput identification of deep intronic splice-disrupting variants using a massively parallel minigene splicing assay
Anabel Lee Martinez Bengochea, John C. Means, and Scott T. Younger
A rare disease is defined as those that affect fewer than 1 in 2,000 individuals. There are about 7,000 rare diseases, which more than 90% of them have no treatment and 50-75% affects children. RNA splicing is the process by which introns are removed, and exons joined together in pre-mRNA processing. Genetic variants within introns can influence RNA splicing, leading to disease through the loss of protein expression and/or function. However, the molecular consequences of deep intronic variants are challenging to predict. We have developed a massively parallel minigene splicing assay that can experimentally detect variant-induced splicing aberrations. The assay consists of a GFP minigene reporter containing a short human intron. Centered within the intron of the reporter gene is a cloning cassette that can be used to insert intronic sequences of interest. We generated a library of 12,400 sequences corresponding to 620 rare genetic variants detected within introns of undiagnosed rare disease patients enrolled in the Genomic Answers for Kids program. We introduced the library into HEK293T cells and evaluated splicing outcomes using a high-throughput sequencing-based strategy. We found that 2.5% of variants profiled gave rise to novel splice acceptor sites and 7% of variants profiled gave rise to novel splice donor sites. We are currently in the process of validating these splicing defects in patient-derived cell models. The approach we describe here has the potential to significantly improve the ability to detect pathogenic splice-disrupting variants in rare disease genomes.
-

Impact of Medical Improvisation Training on Medical Students’ Experience with Communication on Clinical Rotations
Stephanie Kukora, Brittany Batell, Nithin Ravi, Brian J. Zikmund-Fisher, Christopher Thompson, and Patricia Mullan
Effectively preparing students to communicate with patients, families, and teams is a challenge in medical education. Although techniques from Medical Improvisation (MI) have been proposed to teach communication skills in this context, limited evidence exists regarding how MI training impacts real-life interactions.
To provide an MI-based educational training in the pre-clinical year and gather medical students’ reflections following one year of clinical rotations.
We recruited medical student volunteers to participate in an established curriculum (Watson, 2011), lasting 2 hours per week for 5 weeks, prior to beginning clinical rotations. Participants completed evaluations before and after the course, which included structured and open-ended questions about their experience and self-perceived impact. We conducted semi-structured interviews one year later after students completed core clinical rotations and performed thematic analysis on transcripts.
Results: 23 of 24 recruited students completed the course and surveys. Pre/post-course comparison survey data (Table 1) show significant improvements in reported comfort with different communication situations. 35% of students ranked the course as “above average” and 65% ranked it as “excellent.” 11 students (48%) participated in follow-up interviews. All interviewees reported enjoying the course and would recommend it. Major themes included: “regularly used communication skills” (subthemes: building rapport with patients, building trust with the team, responding when not having answers, and reading body language); “challenging communication skills” (sub-themes: responding to emotions, avoiding jargon, giving serious news, and managing conflict); and “skills improved by MI” (subthemes: flexibility, “Yes-and” approach, accepting mistakes, listening, and confidence in unknown situations). Quotes are reported in Table 2. Few students recalled specific exercises, but many felt MI was helpful to their professional development and gave them “tools” for challenging conversations in real-life practice. They also reported benefits in personal growth/wellness and building friendships. Students suggested repeating MI sessions after clinical rotations and MI for interprofessional collaboration but noted attitude of participants and time constraints as barriers. Quotes are listed in Table 3.
Conclusion: MI shows promise as an enjoyable and effective communication skills training approach for medical students.
-

Indications for Early Surgical Intervention in Adolescents with Salter-Harris II Distal Radius Fractures
Cyrus Etebari, Jonathan Warren, Olivia Pruss, Sricharan Yadali, Vincent Staggs, and Micah K. Sinclair
Introduction:
Currently, there is little information regarding risk factors for failure of nonoperative treatment in Salter-Harris II distal radius fractures (SHII-DRF). Our purpose is to identify predictors of which patients will require acute surgery and which will develop late malunion based on degree of deformity and skeletal maturity.
Methods:
This was a review of SHII distal radius fractures from 2017-2020. Patients between 9 and 18 years of age were included. Outcomes of interest included measurements of initial displacement, displacement post-reduction, and displacement after cast removal. These values were compared between patients who did not undergo surgery, had acute surgery, or had late malunion correction. A Classification and Regression Tree (CART) model was also created to identify predictors of acute surgical intervention.
Results:
271 (70% male) SHII distal radius fractures were identified, of which 34 cases (13%) underwent surgical intervention with CRPP or ORIF. Twenty-two (65%) surgical cases were early (median 9.5 days, IQR 3.2-14 days) and 12 (35%) cases were performed to correct late malunion (median 459.5 days, IQR 325.5-542 days). No patients who underwent acute surgery developed malunion. A significantly greater proportion of patients in the late malunion group had dorsal angulation post-reduction compared to the nonoperative group (58% vs. 29%, p=0.048). Similarly, the magnitude of post-reduction tilt was significantly greater in the late malunion group compared to the nonoperative group (median 9, IQR 5-12 vs. median 3, IQR 0-11, p=0.042). Late malunion patients were also significantly older than patients who had successful nonoperative treatment (median 13.7 years vs. median 12.2 years, p=0.038). This information can be found in Table 1. The CART model correctly classified 94% of acute surgery patients with a sensitivity of 55% and specificity of 97%. The CART classification tree and predictors of early surgical intervention can be found in figure 1.
Conclusion:
In SHII distal radius fractures, persistent dorsal angulation after casting was associated with late malunion. Increased Sander’s class and magnitude of deformity in all planes following closed reduction and casting were associated with acute surgery. Treatment guidelines for surgical intervention of this fracture type based on skeletal maturity are limited and this study is among the first to describe treatment that considers skeletal age. These cutoff values for degree of deformity and skeletal maturity can be used to predict need for acute surgery.
-

Interaction between Crk and β-III spectrin during brain development and neurodegeneration
Shufei Zhuang, Jay L. Vivian, David K. Johnson, Lance Rodan, Tom Curran, and Taeju Park
Brain development involves a combination of neuronal proliferation, migration, differentiation, neurite projections and synapse formation, to establish a complex neural network. Defects in these processes can lead to severe developmental abnormalities in children, including neurodegeneration, and formation of brain tumors. SPTBN2, which encodes β-III spectrin, is mutated in spinocerebellar ataxia type 5 (SCA5), a neurodegenerative disorder resulting in uncoordinated gait, limb and eye movements, and slurred speech. Mice deficient in β-III spectrin develop a SCA5 phenotype in an age-dependent manner, including gait abnormality, tremors, cerebellar atrophy, and Purkinje cell loss. Previously, we demonstrated that mice lacking both Crk and CrkL in neurons display significant defects in brain development, including cerebellar hypofoliation, failure of Purkinje cell migration, impaired dendritic development, and disruption of layer formation mediated by the Reelin pathway.
Recently, exome sequencing of a child with a severe global developmental delay, poor growth, and ataxia revealed compound heterozygous mutations in CRK (a truncation mutation: CRK-R88X) and SPTBN2 (a point mutation: SPTBN2-M136V). The siblings carried the same mutation in SPTBN2, but they were asymptomatic. We hypothesize that the interaction between Crk and β-III spectrin is important for brain development and that β-III spectrin lies downstream of Crk in the Reelin signaling pathway.
Three-dimensional molecular modeling indicated that the truncation mutation CRK-R88X renders the Crk protein unstable and inactive. Both β-III spectrin and Crk proteins were detected in mouse embryonic cortical extracts by Western blot analysis. We generated single heterozygous mutant mice for CRK-R88X and SPTBN2-M136V, respectively, and crossed them to generate double heterozygous mice. The double heterozygous mice did not exhibit weight loss or ataxia at 2 months. Hematoxylin and eosin staining of 2-month-old double mutant mouse brains did not show any gross anatomical defects. We plan to carry out immunohistochemistry analysis to determine further details of brain development in these mice. We will also examine motor coordination changes using behavioral test instruments for potential neurodegeneration associated with aging.
Our goal is to determine whether the clinical findings are recapitulated in our mouse models. Results obtained from the mouse models would provide insights into the interaction between Crk and β-III spectrin during brain development and neurodegeneration.
-
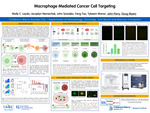
Macrophage Mediated Cancer Cell Targeting
Molly Leyda, Jacqelyn Nemechek, John Szarejko, John M. Perry, and Douglas Myers
Macrophages are a diverse and widespread type of innate immune cell which play an important role in homeostasis and defense. In a process called phagocytosis, macrophages engulf dying cells, foreign substances, and pathogens. Importantly, macrophages can present antigens from phagocytosed cells allowing them to initiate an adaptive immune response against remaining cells of the same type. Despite the immunosuppressive nature of the tumor microenvironment, macrophages often infiltrate tumors where they can either promote or inhibit cancer development, though the specific conditions influencing their pro- vs anti-cancer activity remain enigmatic. Recently, macrophages have been brought into the spotlight of immunotherapy research due to the hope of harnessing their ability to migrate into tumors, phagocytose cancer cells, and mobilize an antitumor T-cell response. However, questions remain about how macrophages recognize, or fail to recognize, cancerous cells for clearance, and how they can promote vs inhibit tumor progression.
To identify modulators of macrophage activation, we have developed a model to visualize and quantify phagocytosis. In this model, bone marrow-derived macrophages are stained with CMFDA, a green cell tracker dye. Cancer cells are stained with pHrodo red, a pH sensitive fluorogenic probe which is designed to fluoresce brighter when inside the acidic phagosome, indicating phagocytosis has occurred. Macrophages are co-cultured with the cancerous target cells then imaged and analyzed. Phagocytosed cells can be visualized through fluorescence microscopy and the number of fluorescent engulfed cells quantified with flow cytometry. This in vitro model allows us to test how macrophages differentially engulf target cells based on various conditions such as macrophage polarization state or cancer cell phenotype. Data acquired from these experiments helps us delineate which characteristics of cancer cells are recognized by macrophages allowing us to better understand the role of phagocytosis in cancer. Future studies will test modified macrophage states in our tumor models and determine how polarization can be exploited to alter the spectrum of pro- and anti-cancer macrophage activities.
-

Neighborhood Environments and Childhood Obesity in the Kansas City Region
Chelsea Steel, Lauren Fitzpatrick, Qianxia Jiang, Robin Shook, Ann M. Davis, Sarah Hampl, and Jordan A. Carlson
Background: Neighborhood environments are known to impact health behaviors, but little data are available to support local decision making in the Kansas City region.
Objective: This project investigated childhood obesity rates across neighborhoods in the Kansas City metropolitan area and associations with four neighborhood environment characteristics: walkability, parks, healthy food access, and poverty.
Methods: Using Children’s Mercy primary care patient data from ~20,000 children ages 6-17 (2017-2020), obesity rates were calculated and mapped for all census tracts in the 6-county Kansas City region with ≥15 patients. Publicly available socioeconomic and built environment data were integrated to investigate associations and map co-occurrences of childhood obesity with the four neighborhood characteristics. Park quality was measured using observational audits. Mixed effects regression models were used to test associations and were adjusted for sociodemographics.
Results: The association between greater walkability and lower BMIz was specific to 9–17-year-olds (B=-0.03 [95% CI=-0.06, 0], p=.033). Children living in one of the 25% highest walkable census tracts were 7% less likely to have obesity than those living in one of the 25% lowest walkable tracts. A greater number of parks was associated with a lower BMIz (B=-0.02 [-0.04, -0.01], p=.020). Children living in a census tract with 3 or more parks were 7% less likely to have obesity than those living in a tract with 0 parks. Children whose nearest park had better overall park quality were less likely to have obesity (OR=0.94 [0.89,0.98], p=.034) and this association was strongest among 12–14-year-olds, girls, and higher income neighborhoods. Healthy food access was not associated with BMIz or obesity. Large differences were observed in obesity rates by neighborhood poverty. Children living in one of the 25% lowest poverty census tracts were 20% less likely to have obesity than those living in one of the 25% highest poverty tracts.
Conclusions: These data show a clear link between neighborhood environment characteristics and childhood obesity in the Kansas City region, revealing health inequities that are based on where a child lives. Children in the region are less likely to have obesity if they live in a neighborhood that has high walkability, high park access, and/or a moderate-to-low rate of poverty. There are many areas of the city where high poverty, low walkability, and low park access co-occur. Multiple sectors must work together and strive for ambitious community transformations to combat the existing environmental health disparities in the region.
-

Overexpression of Crk and CrkL Increases the Motility of High-Grade Glioma Cells
Neka Large and Taeju Park
Background: Glioblastoma and diffuse intrinsic pontine glioma (DIPG) are high-grade gliomas, and their diffuse invasion into neighboring healthy brain tissues contributes to recurrence and dismal treatment outcomes. The expression levels of CT10 regulator of kinase (Crk) and Crk-like (CrkL) are elevated in many human cancers, including glioblastoma and DIPG. Elevation of Crk and CrkL leads to poor prognosis, and they have been proposed as therapeutic targets for glioblastoma. Recently we used gene knockdown to demonstrate that Crk and CrkL are required for the motility of glioblastoma and DIPG cells. Here we used synthetic messenger RNA (mRNA) to investigate the effects of Crk and CrkL overexpression on the motility of glioblastoma and DIPG cells.
Methods: We synthesized mRNA in vitro and electroporated a human glioblastoma cell line, U-118MG, and a human DIPG cell line, SF8628 with mRNA to induce overexpression of Crk and CrkL. Then we determined the respective, quantitative contributions of Crk and CrkL to cellular functions. Impedance-based, real-time measurements of tumor cell adhesion, migration, and invasion were performed using the xCELLigence Real-Time Cell Analyzer (Agilent).
Results: Transfection with CrkII, CrkI, or CrkL mRNA led to an mRNA concentration-dependent expression of exogenous CrkII, CrkI, and CrkL in glioblastoma and DIPG cells. Crk and CrkL overexpression stimulated cell migration for both cell lines, and the stimulation correlated with the Crk and CrkL protein levels. On the other hand, the effect of Crk and CrkL overexpression on cell morphology or proliferation was minimal or modest for both glioblastoma and DIPG cells.
Conclusion/Significances: Our results demonstrate that Crk and CrkL overexpression increases the motility of high-grade glioma cells. Together with our previous study using gene knockdown, these results indicate that the protein levels of Crk and CrkL are critical regulators of glioma cell motility. Our study suggests that the increased motility of the tumor cells may accelerate the infiltration of glioma cells to healthy brain tissues, leading to poor prognosis for Crk/CrkL-overexpressing patients. Therefore, Crk and CrkL may be crucial therapeutic targets for blocking diffuse invasion of high-grade gliomas to improve the efficacy of the standard of care.
Support: Masonic Cancer Alliance Partners Advisory Board grants from Children’s Mercy Hospital (CMH) and the University of Kansas Cancer Center (KUCC) (to TP), and Natalie’s A.R.T. Foundation (to TP).
-

p53 genetic sensor system to identify novel mutant p53 reactivators
Mrinalini Bhosale, Alejandro Parrales, Mohamed A.A. Alalem, Atul Ranjan, Elizabeth Thoenen, and Tomoo Iwakuma
Tumor suppressor Tp53 is the most common mutated gene in human cancers. Missense mutations on the DNA binding domain of p53 frequently abrogate its tumor suppressor activities. However, wild type p53 (wtp53) activity can be restored of mutant p53 (mutp53) proteins by lowering temperature, insertion of second mutations, and small molecules or peptides. To identify novel compounds that can reactivate wtp53 activities from mutp53, we generated H1299 (p53-null) cells expressing a genetic sensor for wtp53 transcriptional activity. This genetic sensor system consists of two constructs: one containing the GFP gene controlled by SCD1 promoter, which is transcriptionally repressed by wtp53, while the second construct uses the p53-regulated p21 promoter to drive expression of GFP shRNA. Using this sensor, we performed a high-throughput screening of 29,440 compounds and identified two top candidates which specifically reduce GFP expression in p53R175H-expressing cells but not in control p53-null cells. Moreover, these compounds restore wtp53-like conformation of p53R175H and p53R156P proteins and reduce viable cell proliferation on cells with p53R175H when compare with those having wtp53 or p53-null status. These compounds increase the levels of p21, Puma, Bax2 and many more downstream targets of p53 contributing to increase in the transcriptional activity. Since p53 is mutated in more than 50% of human tumors, completion of this study could contribute to develop novel therapies for mutp53-expressing cancers. P53 shows transcriptional activity in its dimeric and tetrameric form. Upon reactivation due to accumulated mutant p53, the wild type converted p53 has lower probability to form a homo-tetramer or homodimer hence its transcriptional activity is hindered. This phenomenon is called dominant negative effect. To address this effect a combination of degrading agent and reactivator should be employed for efficient transcriptional activity. Degrading agents like HSP90 inhibitors or statins can be combined with promising reactivators. We investigated a efficient combination of degrading agent and reactivators for higher transcriptional activity.
-

Premature Pubarche in Prader-Willi Syndrome: Potential Predictors and Consequences
Emily Griffing, Kelsee Halpin, Brian R. Lee, and Emily Paprocki
Objectives: Children with Prader-Willi Syndrome (PWS) may develop premature pubarche (PP). We studied the incidence of PP and potential precursors and consequences.
Methods: A chart review of children with PWS treated at Children’s Mercy Hospital between 1990 – 2021 was performed. Patients not seen in endocrine clinic or without documentation of pubarche were excluded. PP was defined as Tanner stage 2 (TS2) pubic hair in girls < 8 and boys < 9 years old. Gonadarche was defined as having TS2 breast development or testicular volume ≥4 mL. Bone age (BA) divided by chronological age (CA) was used as an index for BA advancement. Homeostatic Model Assessment for Insulin Resistance (HOMA-IR) was calculated as (Fasting insulin, uIU/mL)*(Fasting glucose, mg/dL)/405. Small for gestational age (SGA) was defined as birth weight less than the 10% for age. T2D was defined as having a HbA1c ≥6.5%. Wilcoxon rank-sum, Fisher’s exact, and Kendall rank correlation coefficient (CC) were used.
Results: Analysis included 43 children with PWS, 23 (53.4%) with PP and 20 (46.5%) with normal pubarche (NP). Average age of pubarche was 6.48 ± 0.92 years in PP group and 9.9 ± 1.59 years in NP group. Three patients in PP group and one patient in NP group were treated for central precocious puberty with gonadotropin releasing hormone agonist therapy, but median age at gonadarche did not differ between the groups. No significant differences in sex, race, mutation type, or SGA status existed between groups. Age at pubarche was not correlated with age of rhGH initiation, BMI z-score, or HOMA-IR at pubarche. BMI z-score at pubarche was modestly correlated with degree of pubarchal BA advancement (CC=0.311, p=0.033), but the correlation with difference between final and target height was non-significant (CC=-0.081, p=0.68). Highest HbA1c after pubarche was in the pre-diabetes range at 5.8% [IQR 5.6, 6.1] in PP group and 5.6% [IQR 5.4, 6.0] in NP group (p=0.356), though frequency of T2D after pubarche did not differ between groups. Those with PP were more likely to have a lower HDL (p=0.041). The difference between target and final height did not differ between groups (p=0.507).
Conclusion: Premature pubarche is common in PWS but does not impact discrepancy from final height, though obesity at pubarche results in advanced bone age. Obesity and insulin resistance may not be the cause of premature pubarche in children with PWS, contrary to what has been seen in obese children without PWS.
-

Prevalence of COVID-19 Infections in Kansas City Children Enrolled in the New Vaccine Surveillance Network
Micah McGlaughlin, Anjana Sasidharan, Dithi Banerjee, Mary Moffatt, Jennifer Schuster, Gina Weddle, Kirsten Weltmer, and Rangaraj Selvarangan
Background: Following the initial COVID-19 outbreak and lockdown of 2020, the SARS-CoV-2 Omicron Variant spread and peaked through the United States December 2021 to February 2022 (CDC, 2023). Hospitalization rates for children, particularly infants to 4 years, peaked during January 2022 with rates higher than in the initial outbreak in 2020 (CDC, 2023). The objective/aim of this study was to determine the rate of SARS-CoV-2 infections in subjects enrolled in a surveillance project in the Emergency Department (ED), Inpatient (IP), and Clinic during Jan 2022 to Dec 2022.
Methods: Patients 18 years and younger with respiratory illness symptoms were enrolled in the CDC’s New Vaccine Surveillance Network (NVSN) study. Respiratory samples, either a mid-turbinate nasal swab collected by enrollers or nasopharyngeal swab collected by clinical providers for standard of care testing (SOC). Each research specimen underwent an EasyMag extraction. Samples from any subject who did not have a standard of care COVID-19 result were tested by Hologic Panther or underwent PCR testing to retrieve the Ct value. All COVID-19 positive specimens without a Ct value also underwent PCR testing to determine the viral load. Demographics, location, monthly distribution were recorded for SARS-CoV-2 positive patients to better understand the epidemiology.
Results: In 2022, the total specimens included in this study was 2,178 with 169 COVID-19 positives for an 8% positivity rate for the year. A higher prevalence of COVID-19 was seen in January with a 38% positivity rate [65/172], Table 1. Most COVID-19 positive cases were seen in age groups 0-1 year and 2-4 years with 40% and 20% respectively, with higher percentage of infections seen in females [51%, 86/169]. The three most common symptoms experienced of COVID-19 positive patients were fever [104/169], cough [99/169], and nasal congestion [50/169]. There were noticeably higher rates in the summertime during July [14/111] and August [25/163].
Conclusion: The continuous surveillance and data analysis of COVID-19 cases at CMH equips Kansas City communities and healthcare systems to deal with a future spike in cases. Our monitoring enables the CDC to receive information regarding COVID-19 cases in the Kansas City area in addition to the data they receive from other collaborating children’s hospitals across the country.
-

Psychometric Properties of a Theory-Based Assessment of mHealth Acceptability in a Faith-based COVID-19 SMS Intervention
Frank T. Materia, Jannette Berkley-Patton, Jenifer Allsworth, Carole Bowe Thompson, Turquoise Templeton, Cassandra Wainright, Makayla Patton, Kathy Goggin, and Delwyn Catley
Design and implementation of mobile health (mHealth) interventions that are usable and acceptable requires assessment of end-users’ perspectives, but theory-based validated measures are scant. Objective: To examine the internal consistency of a novel measure of mHealth acceptability that is being utilized in a COVID-19 testing intervention with African American church members. Methods: Participants completed a novel mHealth acceptability survey measure based on the Theory of Planned Behavior and the Technology Acceptance Model before receiving a religiously-tailored text messaging intervention component to encourage COVID-19 testing. The 7-item scale assessed multiple dimensions of acceptability of text messaging: interest, difficulty, enjoyment, confidence, utility, worry, and likelihood of reading the text messages. Difficulty and worry items were reverse coded. Results: 1040 participants (79% Female, M age=50.5 yrs, 96.8% African American, 26.1% with Bachelor’s degrees) completed the scale. Internal consistency was acceptable (Cronbach’s α=.76), and removing the “difficulty” and “worry” items increased α to .89. Acceptability ratings (utilizing a 5-point scale, with 1=not at all, 5=very) were above the midpoint for all dimensions. Means and standard deviations (±) were: interest (3.27±1.28), difficulty (4.20±1.18), enjoyment (3.05±1.22), confidence (3.80±1.29), utility: (3.43±1.24), worry (4.19±1.20), and likelihood (3.60±1.27). Principal components analysis revealed two components; with the two negatively worded items (“difficulty” and “worry”) forming the second factor. Conclusion: The measure demonstrates promise for assessing baseline acceptability of mHealth intervention components. Generalizability of these findings to other groups and mHealth tools, and future direction for measure development and dissemination, are discussed.
-

Purple zone: a preventative initiation to address elevated BMI for age in people with cystic fibrosis. A pediatric care center practice
Audrey Snell, Shannon Paseka, and Jasmine Sickel
Background:
Nutrition and growth challenges in children with cystic fibrosis (CF) are well-documented. However, in the past decade, a dramatic shift in CF care with more people with CF (pwCF) eligible for highly effective CF transmembrane conductance regulator (CFTR) modulators. Reviewing the Cystic Fibrosis Foundation Patient Registry (CFFPR) in 2021, it was clearly indicated that more than forty percent of adults with CF (awCF) met criteria for overweight or obese based on the Center for Disease Control and Prevention (CDC) definitions for adult overweight/obesity. The percentage of overweight/obese awCF has tripled in the past two decades. In general pediatrics, overweight and obese children are more likely to stay obese into adulthood. Since obesity affects one in five children and adolescents in the United States, the CF team at Children’s Mercy recognized the need to change our approach.
Objective:
The goal of this quality improvement (QI) initiative was to create a standard process to ensure information provided to families on growth and nutrition was consistent among all CF care team members across all nutrition statuses, malnutrition or overweight and obese.
Design/Methods:
Our CF nutrition committee created a nutrition risk algorithm and interventions for color coded groups in October 2018. The groups defined as red, yellow, and green zones for BMI for age < 25%ile, between 25-50%ile, and greater than 50%ile accordingly. In September 2020, we implemented purple zone with BMI for age > 85%ile aligned with CDC categories for pediatric overweight/obesity. During each pre-clinic huddle, yellow, red as well as purple zones patients were identified and followed closely by the dietitians according to the algorithm.
Results:
Fifty two percent patients met the goal of BMI > 50%ile in 2022. The percentage of patients in overweight/obese category, purple zone, has declined from 20% in 2020 down to 13% in 2022. Care givers and patients have better understanding of their nutrition status in colorful ways.
Conclusion:
Implementing the nutrition risk algorithm has strengthened our team’s efforts to improve patient nutrition status. The addition of purple zone brought awareness of being overweight or obese for pwCF. Standard nutrition language used by all CF team members has fostered more consistent communications to patients and families.
-

Qualitative Insights from Physical and Mental Health Providers in Pediatric Integrated Health Care Settings
Nikolaus Schuetz
Background:
It is widely accepted that the mind and the body are connected, so it is critical to better understand the connection in order to improve the healing process, quality of care, and well-being. Integrated care is associated with improved patient outcomes and is well-positioned to address conditions with known comorbidities (such as chronic health conditions and depression/anxiety), serve people who use primary health care providers for mental health needs (especially racial/ethnic minorities), and address the impact mental health can have on physical health trajectories and outcomes. However, there is disagreement regarding how to best combine treatments. There are more than 150 different definitions of integrated health care in the literature, demonstrating there is no consensus for how to best combine physical and mental health care.
Methods:
This qualitative dissertation study is designed through the constructivism paradigm lens, and theoretically grounded in the Biopsychosocial Model and the Common Elements and Common Factors Framework. Case study methodology is used to examine the insight of both mental health and physical health providers, who treat the same patients with a chronic condition in six pediatric clinics: cardiology clinic, cystic fibrosis clinic, diabetes clinic, eating disorder clinic, epilepsy clinic, and pain clinic. Thirteen interviews were conducted with medical doctors, nurse practitioners, psychologists, and social workers. The interviews were recorded, transcribed, coded, and analyzed.
Findings and Discussion:
The analysis resulted in three main themes: the mind and the body are inextricably intertwined, silos: structural impediments to combined care (common elements), and the relationships and approaches that reflect the intertwined connection (common factors). The clinics had varying levels of combined care, including the type and amount of formal mental health treatment provided in the clinic (e.g., psychotherapy), a range of communication protocols, and degree of treatment integration. All participant providers agreed that most or all health conditions would benefit from a higher level of combined care. Unexpected findings include adherence as a novel pathway to illustrate the mind-body connection, clinical social workers provide covert mental health treatment in circumstances when formal treatment is not possible, and the relationships the providers have with the families and with other providers can be just as important as the relationship with the patient.
Conclusion:
The dissertation concludes with strengths, limitations, implications for both mental health and physical health providers, clinics that provide combined care, hospital administrators and leadership, and policy recommendations.
-
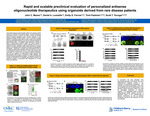
Rapid and scalable preclinical evaluation of personalized antisense oligonucleotides using organoids derived from rare disease patients
John C. Means, Daniel A. Louiselle, Boryana Koseva, T Pastinen, and Scott T. Younger
The generation of patient derived iPSCs has revolutionized the field of personalized medicine. With the unlimited capacity to self-renew and the ability to differentiate into any cell type, iPSCs hold great promise to develop cell based personalized therapies for rare diseases. Antisense oligonucleotides (ASOs) have emerged as a promising therapeutic approach for the treatment of various diseases; and several ASOs for rare diseases have received clinical approval, confirming the potential of this approach. With the advancement of next generation sequencing technologies, the ability to identify disease variants that could benefit from ASO therapeutics has grown. To take advantage of these technologies, we have developed a platform to expediate the rapid characterization of preclinical ASO leads using our iPSC pipeline. We developed an efficient and scalable iPSC pipeline that allows for the rapid generation of iPSCs from patient PBMCs that can be completed in 4-6 weeks. Our reprogramming success rate is >90%, where we can simultaneously generate dozens of iPSCs in parallel, allowing for the generation of >100 patient derived iPSCs in less than 3 months. Using Genomics Answers for Kids (GA4K), we identified a panel of Duchenne muscular dystrophy (DMD) patients that were amendable to ASO therapy. We generated patient derived iPSCs from the DMD panel. In this panel, one patient harbored a structural deletion of exons 46-53 of the DMD gene making it amendable to treatment with the FDA-approved ASO Casimersen. Patient-derived iPSCs treated with ASOs matching the Casimersen sequence showed restoration of Dystrophin protein within 5 days. The DMD panel also included a pair of siblings, both harboring a deep intronic variant in the DMD gene that gives rise to a novel splice acceptor site, incorporation of a cryptic exon, and premature transcript termination. We designed ASOs targeting the intronic variant and observed restoration of Dystrophin protein expression in the patient’s iPSC lines. Next, we differentiated the patient iPSC lines into cardiac organoids and examined organoid function. The cardiac organoids from DMD patients displayed weak arrhythmic contractions and abnormal fluctuations in calcium levels. Treatment with patient specific ASOs before organoid differentiation or post-differentiation, restored both contraction rates and calcium levels comparable to control. Overall, we were able to obtain patient samples, generate patient derived iPSCs, and validate personalized ASOs in fewer than 8 weeks. This platform can be adapted to other cellular models, such as brain organoids, allowing for a rapid and scalable preclinical evaluation of personalized ASOs.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.



